Understanding Conservative Spine Care
Conservative, non‑surgical spine care focuses on relieving pain, restoring function, and preventing progression without incisions. The goal is to reduce inflammation, strengthen supporting muscles, and improve biomechanics through a combination of evidence‑based physical therapy, targeted medications (NSAIDs, muscle relaxants, or limited steroid injections), and activity modification such as ergonomic adjustments and guided exercise. Most specialists recommend a structured trial lasting 6–12 weeks of consistent therapy and medication adherence before deeming the approach unsuccessful. Success is measured by meaningful pain reduction, improved scores on validated tools like the Oswestry Disability Index, and the ability to resume daily activities, work, and sleep without severe limitation. When these milestones are met, patients can often avoid surgery and maintain a higher quality of life.
Red‑Flag Symptoms, Imaging Findings, and Early Warning Signs
| Red‑Flag Symptom | Clinical Sign | Recommended Action |
|---|---|---|
| Neurological deficit | Persistent leg/arm weakness, new numbness, tingling, loss of bladder/bowel control (cauda‑eina) | Immediate MRI/CT and possible emergent decompression |
| Imaging evidence of severe pathology | MRI/CT showing >50% canal narrowing, large disc herniation, foraminal compression; dynamic translation >3 mm or angulation >10° | Correlate with symptoms, consider surgical evaluation |
| Functional decline despite conservative care | Significant drop in Oswestry or Neck Disability Index after ≥6 weeks PT, NSAIDs, activity modification | Discuss surgical referral; reassess treatment plan |
| Severe pain limiting ambulation | Pain prevents walking >100 m, severe positional pain | Obtain imaging, evaluate for stenosis or instability |
| Systemic signs of infection | Fever, elevated ESR/CRP, wound drainage | Urgent work‑up, consider infection‑related surgical intervention |
 When conservative care for back or neck pain fails to produce meaningful relief, clinicians look for red‑flag clues that signal the need for surgical evaluation.
When conservative care for back or neck pain fails to produce meaningful relief, clinicians look for red‑flag clues that signal the need for surgical evaluation.
Neurological deficits that signal urgent evaluation – Persistent leg or arm weakness, new numbness, tingling, or loss of bladder/bowel control (cauda‑eina syndrome)) are emergency findings that require immediate imaging and possible decompression.
Imaging signs of stenosis, disc herniation, and instability – MRI or CT that demonstrates significant canal narrowing, large disc herniation, foraminal compression or dynamic flexion‑extension motion greater than 3 mm translation or >10° angulation correlates with symptoms and predicts failure of non‑operative care.
Functional decline that outpaces conservative improvement – A marked drop in Oswestry or Neck Disability Index scores after an adequate trial of physical therapy, anti‑inflammatory medication, and activity modification indicates that the patient’s quality of life is deteriorating despite optimal conservative treatment.
Questions answered:
- Red‑flag symptoms of spinal stenosis include profound leg weakness, saddle anesthesia, bladder or bowel dysfunction, and severe pain that limits walking.
- When surgery is indicated for L4‑L5 stenosis – after 3‑6 months of failed non‑operative therapy, progressive neuro deficit, or cauda‑eina signs, with imaging showing correlating canal narrowing.
- How to tell if a spinal fusion has failed – Persistent or worsening pain, new radicular symptoms, audible grinding, infection signs, or imaging showing screw loosening or lack of solid bone bridging.
Recognizing these red flags early helps prevent unnecessary delays and guides timely referral to minimally invasive spine surgery when appropriate.
Success Rates, Mortality, and How Often Surgery Is Needed
| Procedure | Approx. Success Rate* | Complication Rate | Mortality (elective) |
|---|---|---|---|
| Thoracic laminectomy (minimally invasive) | 85‑90 % | 7‑12 % | ~0.13 % |
| Lumbar discectomy | 70‑80 % (selected patients) | 8‑15 % | ~0.13 % |
| Lumbar laminectomy (fusion) | 60‑80 % | 10‑20 % | ~0.13 % |
| Multilevel thoracolumbar deformity correction | 55‑70 % | 15‑25 % | 0.2‑0.5 % |
| Overall elective spine surgery | — | 7‑20 % | <0.1 % |
*Success defined as meaningful pain reduction and functional improvement.
 Thoracic laminectomy is a highly effective procedure for isolated spinal stenosis, providing pain and neurologic relief in roughly 85‑90 % of patients. Most individuals (about three‑quarters) report satisfaction at 6‑12 months, especially when the surgery is performed minimally invasively and followed by a structured rehabilitation program.
Thoracic laminectomy is a highly effective procedure for isolated spinal stenosis, providing pain and neurologic relief in roughly 85‑90 % of patients. Most individuals (about three‑quarters) report satisfaction at 6‑12 months, especially when the surgery is performed minimally invasively and followed by a structured rehabilitation program.
Lower‑back surgery—including discectomy, laminectomy, and fusion—yields meaningful pain reduction in 60‑80 % of cases. Success rates climb to 70‑80 % when candidates are carefully selected and adhere to post‑operative therapy, while 20‑40 % may not achieve the desired outcome. Complication rates range from 7‑20 %, and mortality is very low, reported at approximately 0.13 % (≈1 in 1,000) for elective procedures, with lumbar fusion slightly higher at 0.2 % in‑hospital death.
Only about 10 % of people with back pain eventually need surgery; the remaining 90 % recover with conservative care such as physical therapy, medication, and lifestyle changes. Mortality after elective spine surgery remains under 0.1 % overall, though risk increases with more extensive operations or significant comorbidities. Shared decision‑making and a patient‑first approach help ensure surgery is reserved for those who truly need it.
Managing Failed Procedures and Recurrent Symptoms
| Scenario | Imaging Modality | Next Step |
|---|---|---|
| Persistent radicular pain after microdiscectomy (4‑6 weeks) | MRI (look for residual disc, scar, instability) | If inflammation only → PT + NSAIDs + epidural steroid; if compression → revision minimally invasive discectomy or annular closure |
| New back pain with possible hardware issue | CT or X‑ray (hardware integrity) | Evaluate for screw loosening/pseudo‑arthrosis → consider revision fusion or spinal cord stimulation |
| Failed Back Surgery Syndrome (FBSS) | MRI/CT to rule out structural cause | Comprehensive non‑surgical care (graded PT, meds, behavioral therapy, facet blocks); if refractory → spinal cord stimulation |
| Recurrent stenosis after prior decompression | MRI with dynamic sequences | Assess for instability → consider revision decompression with fusion |
| Persistent pain without clear imaging findings | MRI/CT may be negative | Trial of neuromodulation, pain management referral, consider psychosocial interventions |
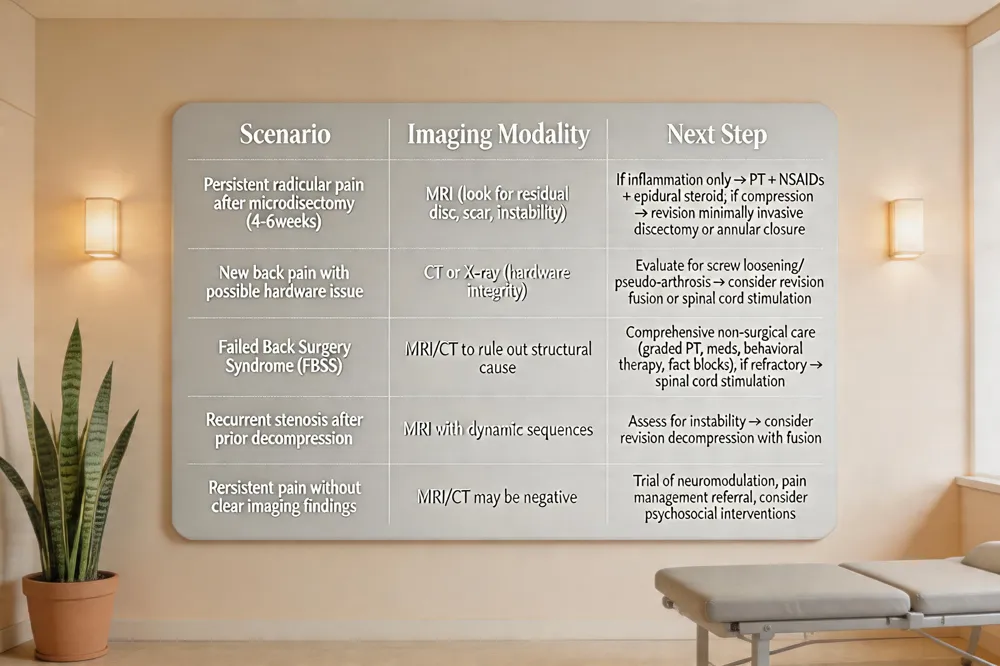 When a microdiscectomy does not bring the expected relief, the first step is repeat imaging—usually MRI or CT—to look for recurrent disc material, scar tissue, or segmental instability (What are the next steps after a failed microdiscectomy?). If only inflammation is seen, a trial of physical therapy, anti‑inflammatory medication, and epidural steroid injections is pursued. Persistent compression may require a minimally invasive revision discectomy, a Barricaid annular closure device, or, in cases of instability, lumbar fusion or total disc replacement.
When a microdiscectomy does not bring the expected relief, the first step is repeat imaging—usually MRI or CT—to look for recurrent disc material, scar tissue, or segmental instability (What are the next steps after a failed microdiscectomy?). If only inflammation is seen, a trial of physical therapy, anti‑inflammatory medication, and epidural steroid injections is pursued. Persistent compression may require a minimally invasive revision discectomy, a Barricaid annular closure device, or, in cases of instability, lumbar fusion or total disc replacement.
Failed back surgery syndrome (FBSS) is addressed initially with comprehensive non‑surgical care: graded physical therapy, targeted pharmacologic control, behavioral therapy, and injections such as facet blocks or radio‑frequency ablation. Neuromodulation with spinal cord stimulation is offered when these measures fail, and revision surgery is reserved for specific anatomic problems like hardware malfunction or pseudo‑arthrosis (How is failed back surgery syndrome treated?).
A microdiscectomy is deemed unsuccessful when pain does not improve after the 4‑6‑week healing window, especially if radiating leg pain, new numbness, weakness, or persistent back pain return, and imaging shows residual disc fragments or scar tissue (How can I tell if a microdiscectomy has failed?).
After spinal stenosis surgery, patients should avoid stairs for the first 2‑3 weeks, then gradually re‑introduce stair climbing with handrails once the incision heals and the surgeon clears them, monitoring for pain or numbness (Can patients walk up stairs after spinal stenosis surgery?).
Non‑Surgical Strategies and Safety Considerations for Older Adults
| Strategy | Description | Benefits / Considerations |
|---|---|---|
| Core‑focused PT | Stabilization, gentle stretching, posture training | Improves support, low injury risk |
| Low‑impact aerobic activity (walking, swimming) | Regular cardio exercise | Enhances overall health, reduces pain |
| Adjunctive modalities (acupuncture, massage, TENS, laser) | Targeted pain relief techniques | May reduce analgesic use, minimal side effects |
| Mind‑body therapies (yoga, tai chi, CBT) | Mindfulness, flexibility, coping skills | Addresses psychosocial factors, improves function |
| Lifestyle modifications (weight loss, smoking cessation, anti‑inflammatory diet) | Nutritional counseling, cessation programs | Decreases mechanical load, systemic inflammation |
| Percutaneous minimally invasive procedures (endoscopic decompression) | Small incisions, local anesthesia | Lower blood loss, shorter stay, suitable for seniors |
 Chronic spine problems in seniors are often managed with a broad, conservative toolkit. Personalized physical‑therapy programs emphasize core stabilization, gentle stretching, posture retraining and low‑impact aerobic activity, while home exercises reinforce gains. Adjunctive modalities such as acupuncture, chiropractic or osteopathic adjustments, massage, laser therapy, TENS, and bio‑feedback can further reduce pain. Mind‑body approaches—including mindfulness, yoga, tai chi, and cognitive‑behavioral therapy—address psychosocial contributors, and lifestyle changes (weight loss, smoking cessation, anti‑inflammatory diet) protect spinal structures.
Chronic spine problems in seniors are often managed with a broad, conservative toolkit. Personalized physical‑therapy programs emphasize core stabilization, gentle stretching, posture retraining and low‑impact aerobic activity, while home exercises reinforce gains. Adjunctive modalities such as acupuncture, chiropractic or osteopathic adjustments, massage, laser therapy, TENS, and bio‑feedback can further reduce pain. Mind‑body approaches—including mindfulness, yoga, tai chi, and cognitive‑behavioral therapy—address psychosocial contributors, and lifestyle changes (weight loss, smoking cessation, anti‑inflammatory diet) protect spinal structures.
Back surgery is avoided when possible because it carries risks that increase with age: infection, blood loss, nerve injury, and the possibility of failed‑back‑surgery syndrome. Conservative care typically yields comparable pain relief without these complications, preserving spinal integrity and reducing long‑term disability.
When surgery is considered for patients 70 years, modern minimally invasive techniques (micro‑discectomy, endoscopic decompression, percutaneous instrumentation) lower blood loss, shorten hospital stays and decrease complication rates. Careful pre‑operative assessment of cardiac, pulmonary and bone health, combined with cement‑augmented screws or other stability‑enhancing devices, makes surgery a viable option for many seniors, offering meaningful pain relief and improved quality of life when non‑operative measures have plateaued.
Expert Surgeons, Recovery Timelines, and High‑Risk Procedures
| Surgeon | Institution | Specialty / Expertise | Notable Techniques |
|---|---|---|---|
| Dr Ehsan Saadat, MD | Cedars‑Sinai (Harvard/Emory training) | Minimally invasive & robotic spine surgery | Robotic‑assisted instrumentation |
| Dr John Rhee, MD | Emory Healthcare | Cervical & lumbar surgery, spinal oncology | Advanced cervical decompression |
| Dr John Heller, MD | Emory Healthcare | Complex cervical deformity | 3‑D navigation for deformity correction |
| Dr Scott Boden, MD | Orthopedic Spine Institute | Spinal oncology, minimally invasive tumor resection | Endoscopic tumor removal |
| Dr Christopher Bono, MD | Orthopedic Spine Institute | High‑outcome spine surgery, innovative care | Multi‑modal pain pathways |
| Dr Sigurd Berven, MD | Orthopedic Spine Institute | Degenerative spine disease, minimally invasive fusion | Cement‑augmented screws |
Recovery Timeline (lumbar fusion example)
- 4‑6 weeks: Light activities, walking, gentle chores
- 3‑6 months: Return to full‑time work, non‑impact exercise
- 6‑12 months: Heavy lifting, high‑impact sports after confirmed fusion
High‑Risk Procedures
- Spinal cord tumor resection
- Complex cervical fusion
- Multi‑level thoracolumbar deformity correction
 When patients reach the point where conservative care no longer relieves pain, they look for a spine specialist with a proven record of success. The most successful surgeons in the United States include Dr Ehsan Saadat, MD, a Harvard‑ and Emory‑trained orthopedic spine expert who pioneered minimally invasive and robotic techniques at Cedars‑Sinai; Dr John Rhee, MD, a leader in cervical and lumbar surgery at Emory Healthcare and former president of the Cervical Spine Research Society; Dr John Heller, MD, also at Emory, renowned for complex cervical deformity work; Dr Scott Boden, MD, a spinal oncology authority known for minimally invasive approaches; and Dr Christopher Bono, MD, and Dr Sigurd Berven, MD, consistently ranked for high patient‑outcome scores and innovative care.
When patients reach the point where conservative care no longer relieves pain, they look for a spine specialist with a proven record of success. The most successful surgeons in the United States include Dr Ehsan Saadat, MD, a Harvard‑ and Emory‑trained orthopedic spine expert who pioneered minimally invasive and robotic techniques at Cedars‑Sinai; Dr John Rhee, MD, a leader in cervical and lumbar surgery at Emory Healthcare and former president of the Cervical Spine Research Society; Dr John Heller, MD, also at Emory, renowned for complex cervical deformity work; Dr Scott Boden, MD, a spinal oncology authority known for minimally invasive approaches; and Dr Christopher Bono, MD, and Dr Sigurd Berven, MD, consistently ranked for high patient‑outcome scores and innovative care.
After a lumbar fusion, most patients can begin light activities—walking, gentle chores—within 4‑6 weeks if post‑operative instructions are followed. By 3‑6 months, many return to full‑time work and non‑impact exercise, while heavy lifting and high‑impact sports are delayed until solid bone fusion is confirmed, usually 6‑12 months after surgery.
The three riskiest spine procedures are: (1) spinal cord surgery such as tumor resection, (2) complex cervical fusion, and (3) multi‑level thoracolumbar deformity correction. These operations carry the highest rates of neurological injury, blood loss, and infection, making careful patient selection and surgeon expertise essential.
Patients at the Orthopedic Spine Institute of St. Louis benefit from this patient‑first model: a thorough trial of non‑operative care, clear communication about risks and benefits, and referral to minimally invasive surgery only when evidence shows that conservative measures have failed.
Taking the Next Step with a Patient‑First Approach
Conservative care is considered unsuccessful when pain persists beyond 6–12 weeks despite physical therapy, medications, and activity modification; when neurological red flags appear, such as progressive weakness, numbness, or loss of bladder/bowel control; when imaging reveals significant stenosis, disc herniation, or instability that correlates with symptoms; or when functional scores (e.g., Oswestry Disability Index) remain markedly impaired. If any of these signs are present, schedule a timely evaluation with a spine specialist. At the Orthopedic Spine Institute of St. Louis, we prioritize shared decision‑making, reviewing all non‑operative options, discussing risks and benefits, and aligning treatment with each patient’s goals before considering minimally invasive surgery.
