Why a Single Home Move Can Make a Difference
The sacroiliac (SI) joint is the body’s largest weight‑bearing joint, linking the sacrum at the base of the spine to the ilium on each side of the pelvis. Though its motion is limited to just a few millimetres of translation and a couple of degrees of rotation, it bears the daily stresses of walking, sitting, and lifting. When the surrounding muscles—glutes, core, hip flexors, and hamstrings—are weak or tight, the SI joint can become irritated, leading to one‑sided lower‑back, buttock, or hip pain that many patients mistake for sciatica. Studies show that roughly 25 % of low‑back pain cases involve the SI joint, and up to 30 % of chronic back pain patients report SI‑related discomfort.
At the Orthopedic Spine Institute of St. Louis we follow a patient‑first, conservative philosophy: we first address the mechanical contributors to pain before considering injections or surgery. Targeted home moves—such as a single knee‑to‑chest stretch, a glute bridge, or a bird‑dog—activate the deep stabilizers that support the pelvis, improve alignment, and reduce joint stress. Even one well‑performed exercise, done consistently, can restore pelvic stability, relieve muscle imbalances, and dramatically lower flare‑up frequency. This low‑risk, evidence‑based approach empowers patients to take control of their recovery while we monitor progress and tailor a full program as needed.
How to Unlock the SI Joint by Yourself
Quick Unlock Routine
| Exercise | Sets / Reps | Duration | Key Cue |
|---|---|---|---|
| Single knee‑to‑chest stretch | 2‑4 × leg | 20‑30 s | Pull knee toward chest, keep opposite hip relaxed |
| Supine hip‑rotation | 2‑3 × side | 8‑12 reps | Bring bent knee across the body, maintain pelvic symmetry |
| Pelvic tilts | 1 × | 10‑15 reps | Flatten lower back against floor, brief hold |
| Glute bridge | 1 × | 8‑12 reps | Lift hips, squeeze glutes, keep spine neutral |
| Side‑plank (knees) | 1 × | 6‑30 s each side | Core engaged, hips level, avoid sagging |
| Dead‑bug | 1 × | 6‑30 s each side | Opposite arm/leg extension, slow control |
 Gentle self‑mobility work can help “unlock” a stiff sacroiliac (SI) joint by reducing compression and restoring muscle balance. Start with a single knee‑to‑chest stretch on a firm surface: pull one knee toward the chest, keep the opposite hip relaxed, and hold for 20–30 seconds; repeat 2‑4 times per leg. Follow with a supine hip‑rotation (bring the bent knee across the body) to promote pelvic symmetry. Add progressive activation moves:
Gentle self‑mobility work can help “unlock” a stiff sacroiliac (SI) joint by reducing compression and restoring muscle balance. Start with a single knee‑to‑chest stretch on a firm surface: pull one knee toward the chest, keep the opposite hip relaxed, and hold for 20–30 seconds; repeat 2‑4 times per leg. Follow with a supine hip‑rotation (bring the bent knee across the body) to promote pelvic symmetry. Add progressive activation moves:
- Pelvic tilts – flatten the lower back against the floor and hold briefly, 10‑15 reps.
- Glute bridge – lift hips while squeezing the glutes, keeping the spine neutral; 8‑12 reps.
- Core stability – dead‑bug or a light side‑plank on the knees, 6‑30 seconds each side. Perform all motions slowly, within a pain‑free range, and stop if discomfort increases. Consistency is key—repeat the routine 3‑5 times daily. For personalized progression and to ensure proper form, consult a physical therapist or spine specialist.
Finding a Trusted SI Joint Exercise PDF
PDF Evaluation Checklist
| Criterion | What to Look For |
|---|---|
| Source | Professional bodies (APTA, NIMH, orthopedic clinics) |
| Content Detail | Step‑by‑step instructions with clear images or video links |
| Exercise Focus | Core stabilization, glute activation, hip abduction/adduction, low‑back mobility |
| Evidence Basis | Includes proven moves (hip thrusts, bridges, bird‑dog, clamshells, piriformis stretch) |
| Authorship | Therapist‑approved or physician‑reviewed |
| Updates | Recent publication date (≤ 3 years) |
| Download Safety | Secure website, no pop‑ups or suspicious links |
 Reputable sources for downloadable exercise guides include professional bodies such as the American Physical Therapy Association, the National Institute of Musculoskeletal Health, and orthopedic clinics that publish therapist‑approved PDFs. When evaluating a PDF, look for clear, step‑by‑step instructions, images or videos that demonstrate proper form, and a focus on core stabilization, glute activation, hip abduction/adduction, and low‑back mobility— all of which are the in evidence‑based SI‑joint programs (e.g., hip thrusts, bridges, bird‑dog, clamshells, and piriformis stretches). The Orthopedic Spine Institute of St. Louis offers a patient‑education PDF that aligns with these principles, guiding users through the single knee‑to‑chest stretch, bridging, bird‑dog, and other core‑strengthening moves. Before beginning any routine, verify that the PDF originates from a trusted health organization and discuss the plan with your therapist or Dr. David S. Raskas to ensure it matches your specific condition. You can download the Institute’s PDF from the “Resources” page or search for “SI joint pain exercise PDF APTA” for additional options.
Reputable sources for downloadable exercise guides include professional bodies such as the American Physical Therapy Association, the National Institute of Musculoskeletal Health, and orthopedic clinics that publish therapist‑approved PDFs. When evaluating a PDF, look for clear, step‑by‑step instructions, images or videos that demonstrate proper form, and a focus on core stabilization, glute activation, hip abduction/adduction, and low‑back mobility— all of which are the in evidence‑based SI‑joint programs (e.g., hip thrusts, bridges, bird‑dog, clamshells, and piriformis stretches). The Orthopedic Spine Institute of St. Louis offers a patient‑education PDF that aligns with these principles, guiding users through the single knee‑to‑chest stretch, bridging, bird‑dog, and other core‑strengthening moves. Before beginning any routine, verify that the PDF originates from a trusted health organization and discuss the plan with your therapist or Dr. David S. Raskas to ensure it matches your specific condition. You can download the Institute’s PDF from the “Resources” page or search for “SI joint pain exercise PDF APTA” for additional options.
Standing Strength Moves for SI Joint Relief
Standing Exercise Summary
| Move | Reps / Steps | Hold | Band? | Primary Target |
|---|---|---|---|---|
| Marching with posterior pelvic tilt | 30‑60 s | – | No | Deep abdominal stabilizers |
| Standing hip‑abduction | 10‑15 × side | 3‑5 s | No | Gluteus medius |
| Monster walks (band around thighs) | 10‑12 steps × side | – | Yes (light) | Glutes & outer hips |
| Side‑lunges (body weight) | 8‑12 × side | – | No | Hip adductors/abductors, glutes |
| Banded squat‑to‑stand (knee band) | 8‑10 reps | – | Yes (moderate) | Whole lower‑body chain, pelvic stability |
 Weight‑bearing drills that keep the pelvis stable are a cornerstone of SI‑joint rehab. Start with simple marching in place while gently pulling the belly button toward the spine to engage the deep abdominal stabilizers and maintain a neutral pelvic tilt. Progress to a standing hip‑abduction: keep the torso upright, lift one leg out to the side, hold 3‑5 seconds, then lower, alternating sides. This isolates the gluteus medius, a key pelvic stabilizer highlighted in multiple therapist‑approved programs.
Weight‑bearing drills that keep the pelvis stable are a cornerstone of SI‑joint rehab. Start with simple marching in place while gently pulling the belly button toward the spine to engage the deep abdominal stabilizers and maintain a neutral pelvic tilt. Progress to a standing hip‑abduction: keep the torso upright, lift one leg out to the side, hold 3‑5 seconds, then lower, alternating sides. This isolates the gluteus medius, a key pelvic stabilizer highlighted in multiple therapist‑approved programs.
Using a light resistance band around the thighs adds activation. Perform small, controlled pelvis rotations or “monster walks” – step side‑to‑side while keeping tension on the band – to further recruit the glutes and outer hip muscles. Begin with 10‑12 steps per side (basic) and advance to longer sets, deeper lunges, or adding a knee‑bend for an intermediate challenge.
Answering the question “SI joint pain exercises standing?”: standing exercises such as marching with posterior pelvic tilt, hip‑abduction, side‑lunges, and banded monster walks specifically strengthen the glutes, hips, and core while maintaining pelvic stability, reducing stress on the sacroiliac joint and alleviating pain.
Gentle SI Joint Exercises for the Elderly
Low‑Impact Routine for Seniors
| Exercise | Position | Reps / Duration | Key Cue |
|---|---|---|---|
| Seated marching | Chair | 30‑45 s | Lift knees, keep spine neutral |
| Heel slides | Supine | 10‑12 reps | Slide heels toward buttocks, avoid arching |
| Seated pelvic tilts | Chair | 8‑10 reps | Tilt pelvis posteriorly, engage core |
| Supported standing hip‑abduction | Chair for balance | 8‑12 × side | Keep torso upright, small lift |
| Chair bridge | Chair or low step | 8‑12 reps | Press heels, lift hips just enough for glute activation |
| Modified bird‑dog (table) | Sturdy table | 6‑8 × side | Extend opposite arm/leg a few inches, avoid lumbar hyperextension |
| Lying clamshells | Firm mattress | 8‑12 × side | Top knee raised, keep pelvis stable |
 Older adults with sacroiliac (SI) discomfort benefit from low‑impact, joint‑friendly movements that avoid heavy loading while still activating the glutes, core and hip stabilizers. Seated options such as marching in place, heel slides, and seated pelvic tilts keep the hips moving without bearing weight, and a supported standing hip abduction (using a chair for balance) gently strengthens the gluteus medius. Bridge variations can be performed from the chair or a low step: sit with feet flat, press through the heels, and lift the hips just enough to feel activation of the glutes and hamstrings while maintaining a neutral spine. A modified bird‑dog can be done from a stable surface—place the hands on a sturdy table, extend one arm and the opposite leg a few inches, hold briefly, then switch sides, keeping the core engaged and avoiding lumbar hyperextension. Clamshells performed lying on a firm mattress with the top knee raised also enhance lateral hip strength. Perform each exercise 8‑12 repetitions, 2‑3 times per week, and increase to daily sessions as tolerated. Stop any movement that provokes sharp pain and consult a physical therapist for personalized progression.
Older adults with sacroiliac (SI) discomfort benefit from low‑impact, joint‑friendly movements that avoid heavy loading while still activating the glutes, core and hip stabilizers. Seated options such as marching in place, heel slides, and seated pelvic tilts keep the hips moving without bearing weight, and a supported standing hip abduction (using a chair for balance) gently strengthens the gluteus medius. Bridge variations can be performed from the chair or a low step: sit with feet flat, press through the heels, and lift the hips just enough to feel activation of the glutes and hamstrings while maintaining a neutral spine. A modified bird‑dog can be done from a stable surface—place the hands on a sturdy table, extend one arm and the opposite leg a few inches, hold briefly, then switch sides, keeping the core engaged and avoiding lumbar hyperextension. Clamshells performed lying on a firm mattress with the top knee raised also enhance lateral hip strength. Perform each exercise 8‑12 repetitions, 2‑3 times per week, and increase to daily sessions as tolerated. Stop any movement that provokes sharp pain and consult a physical therapist for personalized progression.
The Four Power Moves Every SI Joint Patient Should Master
The Four Core Moves
| Move | Sets | Reps | Progression |
|---|---|---|---|
| Bridging variations | 2‑3 | 10‑15 | Single‑leg bridge, add toe‑raise or weight |
| Resistance‑band iliopsoas march | 2‑3 | 10‑15 × leg | Increase band tension, add ankle weight |
| Cat‑camel (spinal mobility) | 2‑3 | 10‑15 cycles | Slow tempo, focus on pelvic neutral |
| Resistance‑band lat‑pull‑down | 2‑3 | 10‑15 | Use heavier band, add core bracing |
 Targeted, low‑impact moves are the cornerstone of conservative sacroiliac (SI) joint care. The four most effective exercises, supported by multiple physical‑therapy handouts and clinical studies, are:
Targeted, low‑impact moves are the cornerstone of conservative sacroiliac (SI) joint care. The four most effective exercises, supported by multiple physical‑therapy handouts and clinical studies, are:
-
Bridging variations – Lie on your back with knees bent, engage the core, and lift the hips until shoulders, hips and knees align. This glute‑bridge activates the gluteus maximus, hamstrings and deep abdominal muscles, providing pelvic stability. Progress to single‑leg bridges or adding a toe‑raise for added challenge.
-
Resistance‑band iliopsoas march – Loop a light band around the foot of the opposite leg, keep hips and knees at 90°, then alternately extend each leg while maintaining a neutral pelvis. This strengthens the hip‑flexor (iliopsoas) group, improving control of pelvic tilt during walking and standing.
-
Cat‑camel (cat‑cow spinal mobility) – On hands‑and‑knees, slowly round the back (cat) and then arch it (camel) while keeping the pelvis neutral. The movement mobilizes lumbar vertebrae, stretches the quadratus lumborum and reinforces deep core engagement, essential for coordinated lumbar‑pelvic motion.
-
Resistance‑band lat‑pull‑down – Hold a band overhead, pull elbows down toward the shoulders, and return under control. This activates the upper‑body stabilizers (latissimus dorsi, trapezius) and the transverse abdominis, helping to maintain proper pelvic alignment.
Perform each exercise for 10‑15 repetitions, 1‑2 times per day, progressing as pain diminishes. Consistent practice of these four power moves improves glute, hip‑flexor, core and upper‑body stability, reducing SI‑joint strain and promoting lasting relief.
Why Workouts Can Ignite SI Joint Inflammation
Inflammation Triggers
| Trigger | Mechanism |
|---|---|
| High‑impact or twisting moves (heavy squats, lunges, rotational sports) | Excess shear & compression → micro‑trauma of joint membrane |
| Muscle imbalances (tight hip flexors, weak glutes/abductors) | Pelvic tilt forward, reduced stabilization → ↑ joint stress |
| Sudden intensity spikes | Lack of gradual adaptation → inflammatory response |
| Poor technique | Improper load distribution → ligament strain |
| Inadequate warm‑up | Muscles stiff, joint less prepared for load |
 When you exercise, the sacroiliac (SI) joint acts as a weight‑bearing hub that transfers forces between the spine and pelvis. High‑impact or twisting movements—such as heavy squats, lunges, or rotational sports drills—create excessive shear and compression, which can micro‑trauma on the joint membrane and surrounding ligaments.
When you exercise, the sacroiliac (SI) joint acts as a weight‑bearing hub that transfers forces between the spine and pelvis. High‑impact or twisting movements—such as heavy squats, lunges, or rotational sports drills—create excessive shear and compression, which can micro‑trauma on the joint membrane and surrounding ligaments.
Common muscle imbalances also play a big role. Tight hip flexors, hamstring or piriformis pull the pelvis forward, while weak glutes, hip abductors (gluteus medius), and deep core muscles (transverse abdominis) fail to stabilize the pelvis. This forces the SI joint to compensate, increasing stress and inflammation.
To protect the joint, adjust your training: prioritize a thorough warm‑up, use controlled, low‑impact progressions, and incorporate targeted strengthening (glute bridges, monster walks, dead‑bug, bird‑dog) and stretching (hamstring, piriformis, supine glute stretches. Maintain proper pelvic alignment and avoid sudden spikes in intensity.
Why does my SI joint keep getting inflamed every time I workout?
The SI joint is a weight‑bearing hub that transfers forces between your upper body and legs, so repetitive or high‑impact movements can overload it with micro‑trauma. When you work out, especially with exercises that involve heavy squats, lunges, or twisting motions, the joint may be subjected to excessive shear and compression, leading to inflammation of the synovial membrane and surrounding tissues. Poor core stability or muscle imbalances—such as tight hip flexors, weak glutes, or over‑active lumbar extensors—can further aggravate the SI joint by forcing it to compensate for the lack of proper support. Additionally, inadequate warm‑up, sudden increases in training intensity, or using improper technique can amplify the stress on the joint, triggering flare‑ups after each session. Addressing these factors with targeted strengthening, flexibility work, and proper biomechanics can help prevent recurrent inflammation and keep your workouts pain‑free.
Progressing to Advanced SI Joint Exercises
Advanced Progression Ladder
| Level | Exercise | Load / Variation | Reps / Sets |
|---|---|---|---|
| Beginner | Hip‑thrusts (body weight) | — | 8‑12 × 3 |
| Intermediate | Single‑leg glute bridge | Add dumbbell on hips | 8‑10 × 3 each leg |
| Advanced | Band‑resisted clamshells | Loop above knees, medium band | 12‑15 × 3 each side |
| Expert | Side‑plank with hip‑abduction | Add light dumbbell on top hip | 30‑45 s × 3 each side |
| Functional | Single‑leg dead‑lift (light kettlebell) | Keep core braced, neutral spine | 8‑10 × 3 each leg |
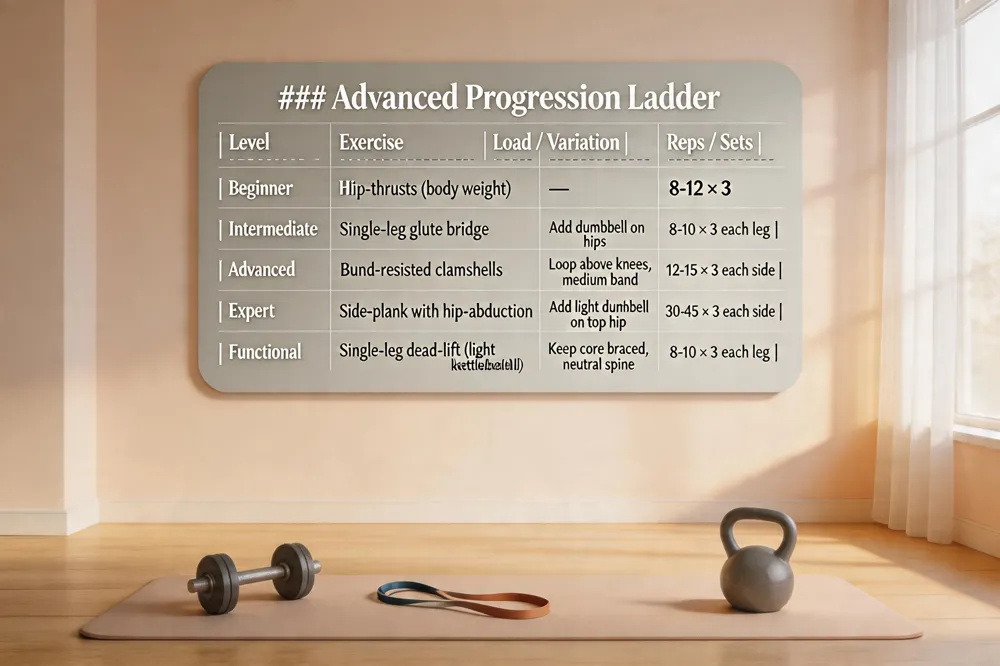 Advanced SI‑joint exercises focus on progressive loading, dynamic stability, and coordinated hip‑pelvic movement. Begin with hip‑thrusts or single‑leg glute bridges, adding weight (dumbbell or barbell) once the body can perform 8‑12 pain‑free. Increase the load gradually and keep the core engaged to protect the lumbar spine. Band‑resisted clamshells and side‑plank variations further target the gluteus medius and outer hip stabilizers; place a resistance loop just above the knees for clamshells and perform side planks from the knees, adding hip‑abduction or a light dumbbell for extra challenge. Functional patterns that integrate core and lower‑body power—such as bird‑dog with a dead‑bug twist, squat‑to‑stand with a knee band, or controlled single‑leg dead‑lifts—train the pelvis to stay stable under real‑world loads. Each movement should be performed slowly, stopped if pain increases, and progressed only after mastering proper form. This systematic approach builds the muscular support needed to reduce SI‑joint flare‑ups and improve overall pelvic stability.
Advanced SI‑joint exercises focus on progressive loading, dynamic stability, and coordinated hip‑pelvic movement. Begin with hip‑thrusts or single‑leg glute bridges, adding weight (dumbbell or barbell) once the body can perform 8‑12 pain‑free. Increase the load gradually and keep the core engaged to protect the lumbar spine. Band‑resisted clamshells and side‑plank variations further target the gluteus medius and outer hip stabilizers; place a resistance loop just above the knees for clamshells and perform side planks from the knees, adding hip‑abduction or a light dumbbell for extra challenge. Functional patterns that integrate core and lower‑body power—such as bird‑dog with a dead‑bug twist, squat‑to‑stand with a knee band, or controlled single‑leg dead‑lifts—train the pelvis to stay stable under real‑world loads. Each movement should be performed slowly, stopped if pain increases, and progressed only after mastering proper form. This systematic approach builds the muscular support needed to reduce SI‑joint flare‑ups and improve overall pelvic stability.
Physical Therapy Blueprint for SI Joint Pain
Blueprint Overview
| Phase | Goal | Sample Exercises | Frequency |
|---|---|---|---|
| Activation | Engage core & glutes | Dead‑bug, bird‑dog, side‑plank (knees) | 3‑5 × wk |
| Strength | Build pelvic stability | Glute bridge, clamshells, monster walks | 3‑4 × wk |
| Progression | Add resistance & dynamic control | Hip‑thrusts, resisted side‑lying leg lifts, banded hip‑abduction | 2‑3 × wk |
| Flexibility | Maintain hip & lumbar mobility | Doorway hamstring stretch (1 min), supine piriformis stretch (15‑30 s), hip‑flexor stretch (15‑30 s) | Daily |
 Physical therapy for sacroiliac (SI) joint pain centers on restoring pelvic stability and mobility through a structured mix of strengthening and stretching. Core stabilization drills such as dead‑bug, bird‑dog, and side‑plank variations teach patients to engage the transverse abdominis and lumbar multifidus while keeping a neutral spine, reducing shear forces on the joint. Glute activation starts with glute bridges and clamshells, then progresses to monster‑walks with a knee‑band and hip‑thrusts that recruit the gluteus maximus, medius, and hamstrings for robust pelvic support. Hip‑abduction advancement follows a similar ladder, moving from side‑lying leg lifts to resisted band abductions. Flexibility is maintained with a targeted stretching protocol: a doorway hamstring stretch (hold 1 minute), a supine piriformis stretch (15‑30 seconds), and a hip‑flexor stretch on each side (15‑30 seconds), all performed slowly and pain‑free. Therapists monitor form, increase repetitions gradually, and incorporate these moves 3‑5 times per week, which research shows can cut pain by up to 68 % within 12 weeks.
Physical therapy for sacroiliac (SI) joint pain centers on restoring pelvic stability and mobility through a structured mix of strengthening and stretching. Core stabilization drills such as dead‑bug, bird‑dog, and side‑plank variations teach patients to engage the transverse abdominis and lumbar multifidus while keeping a neutral spine, reducing shear forces on the joint. Glute activation starts with glute bridges and clamshells, then progresses to monster‑walks with a knee‑band and hip‑thrusts that recruit the gluteus maximus, medius, and hamstrings for robust pelvic support. Hip‑abduction advancement follows a similar ladder, moving from side‑lying leg lifts to resisted band abductions. Flexibility is maintained with a targeted stretching protocol: a doorway hamstring stretch (hold 1 minute), a supine piriformis stretch (15‑30 seconds), and a hip‑flexor stretch on each side (15‑30 seconds), all performed slowly and pain‑free. Therapists monitor form, increase repetitions gradually, and incorporate these moves 3‑5 times per week, which research shows can cut pain by up to 68 % within 12 weeks.
Managing Flare‑Ups and Long‑Term Prevention
Flare‑Up Management Plan
| Step | Action | Details |
|---|---|---|
| 1️⃣ Rest & NSAIDs | Reduce load, control pain | |
| 2️⃣ Gentle activation | Hip thrusts, glute bridges, bird‑dog, clamshells, hamstring stretch | |
| 3️⃣ Frequency | 2‑3 × wk initially, progress to daily as tolerated | |
| 4️⃣ Monitor | Pain > 2 weeks → seek imaging or specialist | |
| 5️⃣ Long‑term habits | Low‑impact cardio, ergonomic seating, balanced diet, avoid tobacco | |
| 6️⃣ Maintenance | Core & glute strengthening (monster walks, dead‑bug, side planks) 3‑5 × wk |
 SI joint flare‑ups typically present as sharp or dull pain localized to the lower back and buttock, often radiating into the hip, groin, thigh, or down the leg. The discomfort worsens after prolonged sitting, standing, stair climbing, or hip rotation, and is accompanied by morning stiffness, a feeling of instability, or occasional clicking. In some cases patients report numbness, tingling, or weakness that mimics sciatica.
SI joint flare‑ups typically present as sharp or dull pain localized to the lower back and buttock, often radiating into the hip, groin, thigh, or down the leg. The discomfort worsens after prolonged sitting, standing, stair climbing, or hip rotation, and is accompanied by morning stiffness, a feeling of instability, or occasional clicking. In some cases patients report numbness, tingling, or weakness that mimics sciatica.
A flare‑up usually lasts a few days to several weeks. When rest, NSAIDs, and gentle physical‑therapy exercises—such as hip thrusts, glute bridges, bird‑dogs, clamshells, and hamstring stretches]—are started promptly, many individuals experience relief within one to two weeks. Persistent pain beyond a few weeks signals the need for further evaluation, possibly including imaging or targeted injections.
Inflammation can resolve, especially when the trigger is acute and addressed early. Acute sacroiliitis often improves with activity modification, anti‑inflammatory medication, and a structured exercise program that strengthens the glutes, core, and hip stabilizers. Chronic inflammatory arthritis may require disease‑specific treatment, but stabilizing the pelvis through regular low‑impact activity (walking, swimming), proper posture, and routine stretching (knee‑to‑chest, piriformis, hamstring) markedly reduces flare‑up frequency.
Long‑term stability hinges on lifestyle habits: maintain a balanced diet, avoid tobacco, stay active with low‑impact aerobic exercise, and use ergonomic seating that keeps the pelvis neutral. Regularly performing the core and glute strengthening moves listed above—hip thrusts, monster walks, dead‑bug, side planks, and quadruped lateral flexion—improves pelvic stability and prevents recurrence. If pain persists despite these measures, consulting an orthopedic spine specialist is essential for tailored care.
Putting It All Together – A Simple Home Routine for Long‑Term SI Joint Health
A daily "knee‑to‑chest unlock" is the cornerstone of any SI‑joint program. While lying on your back, draw one knee toward your chest, keep the lower back flat, and hold for 15‑30 seconds; repeat 2‑4 times per side. This stretch gently mobilizes the hip flexors and lumbar spine, reducing the tension that often pulls the sacroiliac joint out of alignment.
Pair the unlock with a short circuit of core, glute, and hip drills to build the muscular scaffolding that stabilizes the pelvis. Start with a glute bridge (lift hips until shoulders, hips, and knees form a straight line, hold 6 seconds, 8‑12 reps), then move to a bird‑dog (alternate arm‑leg lift, hold 6‑30 seconds, 8‑12 reps per side) and finish with a monster walk (resistance band around the knees, small lateral steps, 10‑15 steps each direction). These movements activate the gluteus maximus, medius, deep abdominal muscles, and hip abductors—exactly the muscles highlighted in multiple clinical sources as vital for SI‑joint support.
If pain persists despite consistent practice, or if you notice new symptoms such as leg weakness, numbness, or worsening stiffness, schedule a review with the Orthopedic Spine Institute. Their team can assess alignment, tailor a progressive exercise plan, and determine whether adjunctive treatments (e.g., manual therapy, injections) are needed to prevent chronic flare‑ups.
