Why Back Injuries Matter in the Workplace
Back injuries are among the most common workplace ailments in the United States—roughly one‑in‑five work‑related injuries involve the back, and lower‑back problems account for about 80 % of those cases. This high prevalence translates into a massive financial burden: workers’ compensation programs spend billions each year on medical care, wage replacement, and disability benefits for uncomplicated low back pain, and recurrent or chronic cases drive costs even higher.
Historically, treatment followed a pathology‑based model that focused on identifying a specific anatomic fault and then surgically correcting it. Recent research, however, shows that a functional restoration approach—centered on ergonomic modifications, core‑strengthening exercise, and coordinated physical therapy—delivers superior clinical outcomes while containing expenses. By prioritizing early, conservative care and workplace‑specific ergonomic advice, insurers can reduce the need for expensive imaging, injections, and surgery, ultimately lowering claim expenditures and helping injured workers return to duty more quickly.
Understanding Workers’ Comp Back Injuries
Key Points
| Diagnosis | Typical Symptoms | Required Documentation |
|---|---|---|
| Lumbar strain/sprain | Pain, stiffness, limited ROM | Physician note linking injury to work activity, imaging if needed |
| Disc herniation | Radiating leg pain, numbness, weakness | MRI/CT showing disc pathology, functional‑capacity evaluation |
| Spinal stenosis | Neurogenic claudication, lower‑extremity weakness | Imaging (MRI) confirming canal narrowing, work‑related aggravating factors |
| Back pain (non‑specific) | Diffuse ache, muscle spasm | Detailed pain diary, employer incident report, qualified medical opinion |
 Back injuries in the workplace most often result from improper lifting techniques, repetitive motions, or slips and falls. The typical diagnoses seen in workers’ compensation claims include lumbar strains or sprains, disc herniations, and spinal stenosis, each producing pain, stiffness, and limited mobility. To qualify for benefits, the injury must be documented by a qualified medical professional as work‑related, reported promptly to the employer, and the claim filed within the state‑specified deadline (often 30‑90 days). Comprehensive medical records, imaging, and a clear link between job duties and the injury are essential for approval.
Back injuries in the workplace most often result from improper lifting techniques, repetitive motions, or slips and falls. The typical diagnoses seen in workers’ compensation claims include lumbar strains or sprains, disc herniations, and spinal stenosis, each producing pain, stiffness, and limited mobility. To qualify for benefits, the injury must be documented by a qualified medical professional as work‑related, reported promptly to the employer, and the claim filed within the state‑specified deadline (often 30‑90 days). Comprehensive medical records, imaging, and a clear link between job duties and the injury are essential for approval.
Conservative Care First: Functional Restoration and Ergonomics
Conservative Care Overview
| Intervention | Goal | Example |
|---|---|---|
| Functional restoration | Restore pain‑free functional activity | Core‑stability program, Pilates‑style exercises |
| Ergonomic modification | Reduce stress on injured structures | Adjust workstation height, lumbar support, proper lifting technique training |
| Low‑impact aerobic conditioning | Improve endurance, promote circulation | Gradual walking or stationary bike program |
| Education & self‑management | Prevent chronicity | Pain‑monitoring diary, activity pacing strategies |
 When a worker sustains a low‑back strain, the most cost‑effective and clinically successful path is a functional restoration program rather than a traditional, pathology‑based approach. Functional restoration focuses on returning the employee to full, pain‑free activity by rebuilding core stability, improving movement patterns, and enhancing endurance, rather than merely treating isolated tissue damage. Early ergonomic recommendations—such as adjusting workstation height, using lumbar support, and teaching proper lifting mechanics—speed healing by reducing undue stress on the injured muscles and discs. A structured exercise regimen that emphasizes coordination (e.g., Pilates‑style core control) and endurance (gradual progression of low‑impact aerobic work) supports tissue healing, prevents chronicity, and ultimately lowers workers’ compensation costs. By prioritizing these conservative measures, clinicians can achieve better outcomes, faster return‑to‑work, and reduced long‑term expenses.
When a worker sustains a low‑back strain, the most cost‑effective and clinically successful path is a functional restoration program rather than a traditional, pathology‑based approach. Functional restoration focuses on returning the employee to full, pain‑free activity by rebuilding core stability, improving movement patterns, and enhancing endurance, rather than merely treating isolated tissue damage. Early ergonomic recommendations—such as adjusting workstation height, using lumbar support, and teaching proper lifting mechanics—speed healing by reducing undue stress on the injured muscles and discs. A structured exercise regimen that emphasizes coordination (e.g., Pilates‑style core control) and endurance (gradual progression of low‑impact aerobic work) supports tissue healing, prevents chronicity, and ultimately lowers workers’ compensation costs. By prioritizing these conservative measures, clinicians can achieve better outcomes, faster return‑to‑work, and reduced long‑term expenses.
When Conservative Care Fails: Minimally Invasive Options
Minimally Invasive Options
| Procedure | Indication | Typical Recovery Time |
|---|---|---|
| Epidural steroid injection | Persistent radicular pain >4‑8 weeks | 1‑3 months pain relief |
| Radiofrequency ablation | Facet‑joint mediated pain | 3‑6 months symptom reduction |
| Micro‑discectomy | Disc fragment causing nerve compression | 2‑4 weeks to return to light duties |
| Endoscopic decompression | Stenosis or disc herniation not responding to injections | 4‑6 weeks for functional improvement |
| Percutaneous vertebroplasty | Osteoporotic compression fracture | Same‑day procedure, ambulation within 24 h |
 If a worker’s back injury does not improve after 4–8 weeks of activity modification, physical therapy, NSAIDs, and chiropractic care, many insurers—including workers’ compensation carriers—allow a transition to minimally invasive interventions. Epidural steroid injections deliver anti‑inflammatory medication directly to irritated nerve roots, often providing pain relief for several months; radiofrequency ablation uses heat to interrupt pain signals from facet joints. When these injections are insufficient, procedural options such as micro‑discectomy, endoscopic decompression, or percutaneous vertebroplasty can be considered. Micro‑discectomy removes a herniated disc fragment under a small incision, while endoscopic decompression expands the spinal canal with a camera‑guided tool, and vertebroplasty stabilizes compression fractures by injecting bone cement. The decision to move from therapy to surgery typically hinges on persistent pain that limits functional activities, imaging that confirms a structural lesion correlating with symptoms, and failure of at least two targeted injection series. Early documentation of these criteria helps secure workers’ compensation authorization and speeds the patient’s return to work.
If a worker’s back injury does not improve after 4–8 weeks of activity modification, physical therapy, NSAIDs, and chiropractic care, many insurers—including workers’ compensation carriers—allow a transition to minimally invasive interventions. Epidural steroid injections deliver anti‑inflammatory medication directly to irritated nerve roots, often providing pain relief for several months; radiofrequency ablation uses heat to interrupt pain signals from facet joints. When these injections are insufficient, procedural options such as micro‑discectomy, endoscopic decompression, or percutaneous vertebroplasty can be considered. Micro‑discectomy removes a herniated disc fragment under a small incision, while endoscopic decompression expands the spinal canal with a camera‑guided tool, and vertebroplasty stabilizes compression fractures by injecting bone cement. The decision to move from therapy to surgery typically hinges on persistent pain that limits functional activities, imaging that confirms a structural lesion correlating with symptoms, and failure of at least two targeted injection series. Early documentation of these criteria helps secure workers’ compensation authorization and speeds the patient’s return to work.
What to Say (and Not Say) to Your Workers’ Compensation Doctor
Communication Tips
| Do | Don't |
|---|---|
| Disclose all prior back issues and surgeries | Lie about prior injuries |
| Describe the incident with specific task, position, and event | Exaggerate pain level or claim cessation of treatment when still in therapy |
| Keep a consistent daily pain and functional‑limitation log | Provide conflicting reports across appointments |
| Provide accurate medication and therapy history | Omit treatments to appear less severe |
 When you meet with a workers’ compensation (WC) physician, honesty and clarity are your most valuable tools.
Honesty about prior injuries and medical history – Disclose any previous back problems, surgeries, or chronic conditions. Insurers often challenge a claim by citing pre‑existing issues, so a complete medical history protects you from accusations of deception.
Accurate description of the workplace incident – Explain exactly how the injury occurred, including the task you were performing, the position you were in, and any sudden event (e.g., lifting a heavy box, a slip, or repetitive twisting). Precise details help the doctor link your symptoms to the work‑related event, which is essential for claim approval.
Consistent reporting of pain and functional limitations – Keep a daily log of pain levels, stiffness, muscle spasms, and any loss of range of motion. Report the same information at each appointment; inconsistencies can be used to argue that your condition is not as severe as claimed.
What to avoid saying – Never lie about prior injuries, exaggerate pain, or claim you have stopped treatment when you have not. Misrepresenting the severity of your symptoms, the cause of the injury, or your treatment adherence can lead to claim denial or loss of benefits.
By staying truthful, detailed, and consistent, you give your WC doctor the evidence needed to support your claim and facilitate a timely return to work.
When you meet with a workers’ compensation (WC) physician, honesty and clarity are your most valuable tools.
Honesty about prior injuries and medical history – Disclose any previous back problems, surgeries, or chronic conditions. Insurers often challenge a claim by citing pre‑existing issues, so a complete medical history protects you from accusations of deception.
Accurate description of the workplace incident – Explain exactly how the injury occurred, including the task you were performing, the position you were in, and any sudden event (e.g., lifting a heavy box, a slip, or repetitive twisting). Precise details help the doctor link your symptoms to the work‑related event, which is essential for claim approval.
Consistent reporting of pain and functional limitations – Keep a daily log of pain levels, stiffness, muscle spasms, and any loss of range of motion. Report the same information at each appointment; inconsistencies can be used to argue that your condition is not as severe as claimed.
What to avoid saying – Never lie about prior injuries, exaggerate pain, or claim you have stopped treatment when you have not. Misrepresenting the severity of your symptoms, the cause of the injury, or your treatment adherence can lead to claim denial or loss of benefits.
By staying truthful, detailed, and consistent, you give your WC doctor the evidence needed to support your claim and facilitate a timely return to work.
Typical Settlement Offers and Compensation Ranges
Settlement Ranges by Injury Type
| Injury Type | Settlement Range (USD) |
|---|---|
| Soft‑tissue strain | $10 k – $50 k |
| Bulging disc | $30 k – $100 k |
| Herniated disc (non‑surgical) | $75 k – $200 k |
| Herniated disc (surgical) | $200 k – $750 k |
| Severe permanent disability | $500 k – $2 M+ |
| Average overall payout | $20 k – $50 k (varies by severity and state) |
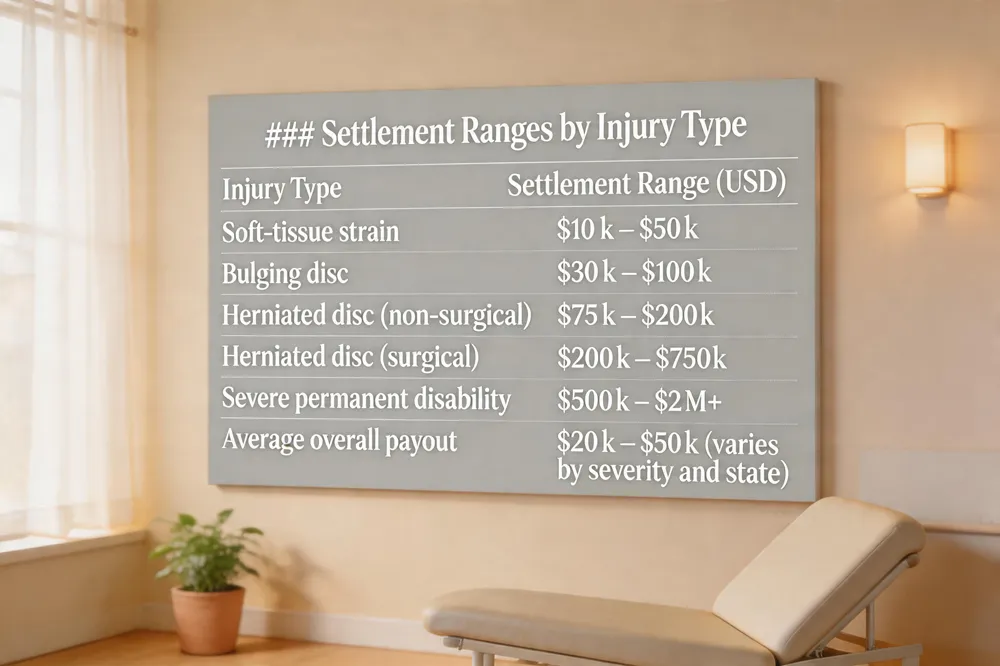 Factors influencing settlement amounts Workers’ compensation settlements depend on injury severity, required medical care, duration of disability, pre‑existing conditions, and state‑specific benefit formulas. A lumbar strain that resolves with conservative therapy usually yields a lower offer, while a herniated disc that needs surgery or results in permanent nerve damage commands a higher figure.
Factors influencing settlement amounts Workers’ compensation settlements depend on injury severity, required medical care, duration of disability, pre‑existing conditions, and state‑specific benefit formulas. A lumbar strain that resolves with conservative therapy usually yields a lower offer, while a herniated disc that needs surgery or results in permanent nerve damage commands a higher figure.
Medical expenses vs. wage loss vs. disability benefits Settlements separate three core components: (1) Medical expenses—past and future costs for imaging, physical therapy, injections, surgeries, and assistive devices; (2) Wage loss—temporary total or partial disability calculated as a percentage of the worker’s average weekly wage; and (3) Disability benefits—permanent partial or total disability ratings that add a lump‑sum or ongoing compensation based on functional loss.
Role of attorney representation An experienced workers’ comp attorney can quantify each component, negotiate with insurers, and counter denial tactics. Studies show represented claimants receive settlements roughly twice as high as unrepresented ones.
What is a typical settlement offer for a back injury? Offers range widely: soft‑tissue strains $10‑$50 k, bulging discs $30‑$100 k, herniated discs $75‑$350 k, and surgeries $200‑$750 k or more. Severe permanent disability can exceed $500 k up to $2 million.
How much can you receive for a back injury suffered at work? The average workers’ comp payout falls between $20 k and $50 k, but serious or permanently disabling injuries can push the total well beyond $50 k when medical, wage, and disability components are combined.
Proving a Back Injury: Evidence and Expert Testimony
Evidence Required for Proof
| Evidence Type | Why Important |
|---|---|
| MRI/CT imaging | Objective visualization of disc/soft‑tissue pathology |
| Specialist report (orthopedic/neurologist) | Professional interpretation linking imaging to symptoms |
| Pain diary & functional‑capacity evaluation | Quantifies severity and work‑related limitations |
| Employer job description & incident report | Shows direct connection between job duties and injury |
| Independent expert witness | Bridges medical findings to legal causation standards |
 Back pain is a symptom, not a disease, so establishing a work‑related back injury often requires objective evidence. Medical imaging requirements: Simple X‑rays may miss soft‑tissue damage; MRI or CT scans are essential for visualizing disc herniations, ligament sprains, and facet‑joint pathology. Specialist reports from a board‑certified orthopedist or neurologist should interpret these images and describe the exact level and severity of the injury.
Back pain is a symptom, not a disease, so establishing a work‑related back injury often requires objective evidence. Medical imaging requirements: Simple X‑rays may miss soft‑tissue damage; MRI or CT scans are essential for visualizing disc herniations, ligament sprains, and facet‑joint pathology. Specialist reports from a board‑certified orthopedist or neurologist should interpret these images and describe the exact level and severity of the injury.
Documenting pain, functional limitations, and work‑related activities: Workers must keep a daily pain diary, note any loss of range of motion, and record how the injury limits specific job tasks such as lifting, bending, or prolonged sitting. Physical‑therapy notes, functional‑capacity evaluations, and employer‑provided job descriptions help translate subjective pain into measurable functional loss.
Using expert witnesses: An independent medical expert can link the documented pathology to the workplace event, explain why the injury would not have occurred outside work, and testify to causation and prognosis. This expert testimony bridges the gap between clinical findings and legal standards.
Answer to the question: Proving a back injury can be challenging because pain is subjective and imaging may be required to reveal hidden soft‑tissue damage. Comprehensive medical records, detailed functional documentation, and a qualified expert witness are key to demonstrating that the injury arose from a specific work‑related incident.
State‑Specific Insights: California and Beyond
State‑Specific Settlement Insights
| State | Typical Settlement Range (USD) | Notable Factors |
|---|---|---|
| California | $10 k – $2 M+ (depends on injury severity) | One‑year filing deadline, 30‑day hearing request window |
| Georgia | <$100 k for comparable injuries | 100 % coverage of medically necessary treatment, fewer caps |
| New York | $50 k – $150 k (non‑surgical) up to higher for surgery | Wage‑replacement & job‑retraining benefits |
| Ohio | Avg. $39 k | No‑fault system, 1‑year filing deadline, 14‑day appeal window |
 In California, back‑injury settlements range widely: a simple lumbar strain typically resolves for $10,000‑$50,000; a bulging disc $30,000‑$100,000; a herniated disc $75,000‑$350,000; surgery for a herniated disc $200,000‑$750,000; and severe spinal or nerve damage $500,000‑$2,000,000+. Compared with other states, Georgia provides 100 % coverage of medically necessary treatment with fewer caps, but average settlements are lower, often under $100,000 for similar injuries. New York offers wage‑replacement and job‑retraining benefits yet settlements hover around $50,000‑$150,000 for non‑surgical cases and rise sharply when surgery is needed. Ohio’s no‑fault system yields settlements averaging $39,000, with a $1‑year deadline to file a First Report of Injury and a 14‑day window to appeal a denial. California workers must file a claim within one year of injury and has a 30‑day deadline to request a hearing on any adverse decision, underscoring the importance of timely documentation and legal counsel across all jurisdictions.
In California, back‑injury settlements range widely: a simple lumbar strain typically resolves for $10,000‑$50,000; a bulging disc $30,000‑$100,000; a herniated disc $75,000‑$350,000; surgery for a herniated disc $200,000‑$750,000; and severe spinal or nerve damage $500,000‑$2,000,000+. Compared with other states, Georgia provides 100 % coverage of medically necessary treatment with fewer caps, but average settlements are lower, often under $100,000 for similar injuries. New York offers wage‑replacement and job‑retraining benefits yet settlements hover around $50,000‑$150,000 for non‑surgical cases and rise sharply when surgery is needed. Ohio’s no‑fault system yields settlements averaging $39,000, with a $1‑year deadline to file a First Report of Injury and a 14‑day window to appeal a denial. California workers must file a claim within one year of injury and has a 30‑day deadline to request a hearing on any adverse decision, underscoring the importance of timely documentation and legal counsel across all jurisdictions.
Navigating the Claims Process: Forms, Appeals, and Legal Help
Claims Process Checklist
| Step | Form / Action | Deadline |
|---|---|---|
| Initial injury report to employer | Employer‑specific incident report | Within days (state‑specific) |
| File workers’ comp claim | State claim form (e.g., WC‑205 in GA) | Usually within 30‑90 days of injury |
| Request pre‑authorization for diagnostics | Form WC‑205 (GA) or equivalent | Prior to imaging/treatment |
| Appeal a denial | Written request for reconsideration → Administrative law judge hearing | 30 days (NY), 14 days (OH) |
| Seek legal representation | Consult workers’ comp attorney | As early as possible to meet deadlines |
 For workers‑comp back injuries, the first step is filing the proper paperwork. In Georgia, Form WC‑205 is used for pre‑authorization of any diagnostic test or treatment; if the insurer refuses, the injured employee may file Form WC‑PMT to request a conference with an administrative law judge. Most states have similar deadline rules—claims must be reported within days (New York) or weeks (Ohio) of the injury, and any appeal must be lodged within the statutory window (30 days in NY, 14 days in OH). When a claim is denied, the appeal process typically begins with a written request for reconsideration, followed by a formal hearing before the state workers‑comp board or a judge. In complex cases—persistent denials, disputed causation, or the need for future medical funding—consulting a workers‑comp attorney is advisable. An attorney can gather medical evidence, file the correct forms on time, and represent the worker in hearings, greatly improving the odds of a successful claim.
For workers‑comp back injuries, the first step is filing the proper paperwork. In Georgia, Form WC‑205 is used for pre‑authorization of any diagnostic test or treatment; if the insurer refuses, the injured employee may file Form WC‑PMT to request a conference with an administrative law judge. Most states have similar deadline rules—claims must be reported within days (New York) or weeks (Ohio) of the injury, and any appeal must be lodged within the statutory window (30 days in NY, 14 days in OH). When a claim is denied, the appeal process typically begins with a written request for reconsideration, followed by a formal hearing before the state workers‑comp board or a judge. In complex cases—persistent denials, disputed causation, or the need for future medical funding—consulting a workers‑comp attorney is advisable. An attorney can gather medical evidence, file the correct forms on time, and represent the worker in hearings, greatly improving the odds of a successful claim.
Your Path Forward with the Orthopedic Spine Institute
At the Orthopedic Spine Institute we put the patient first, weaving together a seamless, coordinated care team that includes Dr. David S. Raskas, orthopedic spine surgeons, physical therapists, pain specialists, and case managers. This interdisciplinary approach ensures every decision—from diagnostic imaging to the choice of conservative therapy or minimally invasive surgery—is based on your unique functional goals and the demands of your occupation.
Booking an appointment is simple: call our dedicated workers’‑comp line or use the secure online portal to request a consult with Dr. Raskas. Our staff will verify your claim, collect initial medical records, and schedule a same‑day intake examination, minimizing delays that can jeopardize claim approval.
Next steps after your initial visit include thorough documentation of the workplace incident, a complete physical and neurological exam, and appropriate imaging (X‑ray, MRI, or CT). From there, we develop a treatment plan that starts with evidence‑based conservative care—activity modification, core‑strengthening physical therapy, and targeted injections—escalating to minimally invasive procedures only when medically necessary. Throughout the process we keep your employer, insurance adjuster, and legal counsel informed, ensuring timely approvals, uninterrupted treatment, and a faster, safer return to work.
