Why a Clear, Patient‑First Perspective Matters
Minimally invasive spine surgery (MISS) has reshaped how surgeons treat lumbar disc herniation. By using small incisions, tubular retractors, microscopes or endoscopes, MISS preserves muscle and ligament integrity, cuts blood loss by up to 80 % and shortens hospital stays to one‑day or outpatient discharge. Hundreds of peer‑reviewed studies involving more than 10,000 patients show pain‑relief outcomes comparable to open surgery while delivering lower opioid requirements and faster return to work.
Despite these advances, patients often encounter myths. Some believe microdiscectomy guarantees a permanent cure or that all back surgeries are identical. In reality, the procedure targets a specific nerve‑root compression, and recurrence rates of 5‑10 % still exist. Others think the surgery is high‑risk; however, serious complications such as dural tears, infection or nerve injury occur in less than 2 % of cases when performed by experienced surgeons.
The Orthopedic Spine Institute of St. Louis embraces a patient‑first philosophy. Every candidate undergoes a thorough clinical exam, MRI confirmation and a documented trial of six to twelve weeks of conservative care before surgery is considered. The team uses minimally invasive microdiscectomy when appropriate, provides clear pre‑operative counseling, and offers a structured postoperative rehabilitation program focused on core strengthening and lifestyle modification. This transparent, evidence‑based pathway builds trust, reduces anxiety, and positions the institute as a reliable partner for lasting spine health.
Understanding Microdiscectomy: Indications, Levels, and Procedure
| Item | Details |
|---|---|
| Indications | Persistent sciatica from lumbar disc herniation after 6‑12 weeks of PT, NSAIDs, epidural steroids, and other conservative care |
| Levels | L5‑S1 – ≤2 cm incision, microscope/endoscope removes fragment compressing S1 nerve root.<br>L4/L5 – Same technique targeting L4 or L5 nerve root; tubular retractor spares paraspinal muscles. |
| Operative Time | Single‑level L4‑L5: 45‑90 min; total hospital stay 0‑2 days (often outpatient). |
| Microdiscectomy vs. Open | Micro: ≤1‑inch incision, less blood loss, lower infection risk, faster functional return, reduced opioid use.<br>Open: larger incision, muscle division, higher blood loss, longer recovery. |
| Educational Resource | Video on Orthopedic Spine Institute website shows step‑by‑step procedure and expectations. |
 Microdiscectomy is a minimally invasive, spine‑sparing surgery performed when 6‑12 weeks of physical therapy, NSAIDs, epidural steroids, and other conservative measures fail to relieve sciatica caused by a lumbar disc herniation. Microdiscectomy L5‑S1 – A ≤2 cm incision over the L5‑S1 level allows a microscope or endoscope to remove the herniated fragment compressing the S1 nerve root, preserving surrounding muscle and ligamentous tissue. Patients typically experience rapid leg‑pain relief and can be discharged same‑day or after an overnight stay. Microdiscectomy L4/L5 – The same technique targets disc material irritating the L4 or L5 nerve root. The tubular retractor spares the paraspinal muscles, resulting in less postoperative pain and a return to light duties within 4‑6 weeks. Operative time – Single‑level L4‑L5 procedures average 45‑90 minutes; total hospital time is usually 0‑2 days. Microdiscectomy vs. open discectomy – Open discectomy requires a larger incision and muscle division, leading to higher blood loss, infection risk, and longer recovery. In contrast, microdiscectomy’s ≤1‑inch incision, microscopic visualization, and tissue‑preserving approach produce shorter stays, lower opioid use, and faster functional return. Educational video – The Orthopedic Spine Institute’s website hosts high‑quality videos showing the small incision, microscope guidance, and step‑by‑step disc removal, helping patients set realistic expectations and understand the procedure.
Microdiscectomy is a minimally invasive, spine‑sparing surgery performed when 6‑12 weeks of physical therapy, NSAIDs, epidural steroids, and other conservative measures fail to relieve sciatica caused by a lumbar disc herniation. Microdiscectomy L5‑S1 – A ≤2 cm incision over the L5‑S1 level allows a microscope or endoscope to remove the herniated fragment compressing the S1 nerve root, preserving surrounding muscle and ligamentous tissue. Patients typically experience rapid leg‑pain relief and can be discharged same‑day or after an overnight stay. Microdiscectomy L4/L5 – The same technique targets disc material irritating the L4 or L5 nerve root. The tubular retractor spares the paraspinal muscles, resulting in less postoperative pain and a return to light duties within 4‑6 weeks. Operative time – Single‑level L4‑L5 procedures average 45‑90 minutes; total hospital time is usually 0‑2 days. Microdiscectomy vs. open discectomy – Open discectomy requires a larger incision and muscle division, leading to higher blood loss, infection risk, and longer recovery. In contrast, microdiscectomy’s ≤1‑inch incision, microscopic visualization, and tissue‑preserving approach produce shorter stays, lower opioid use, and faster functional return. Educational video – The Orthopedic Spine Institute’s website hosts high‑quality videos showing the small incision, microscope guidance, and step‑by‑step disc removal, helping patients set realistic expectations and understand the procedure.
Recovery Timeline and Activity Guidelines
| Week | Goals / Activities | Restrictions |
|---|---|---|
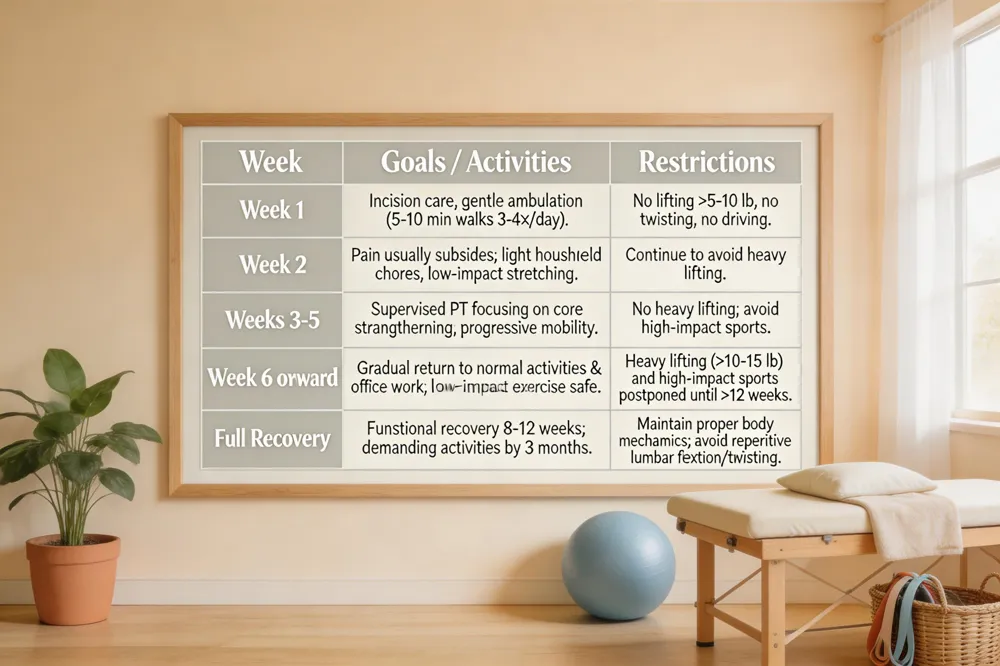
| Week 1 | Incision care, gentle ambulation (5‑10 min walks 3‑4×/day). | No lifting >5‑10 lb, no twisting, no driving. |
| Week 2 | Pain usually subsides; light household chores, low‑impact stretching. | Continue to avoid heavy lifting. |
| Weeks 3‑5 | Supervised PT focusing on core strengthening; progressive mobility. | No heavy lifting; avoid high‑impact sports. |
| Week 6 onward | Gradual return to normal activities & office work; low‑impact aerobic exercise safe. | Heavy lifting (>10‑15 lb) and high‑impact sports postponed until >12 weeks. |
| Full Recovery | Functional recovery 8‑12 weeks; demanding activities by 3 months. | Maintain proper body mechanics; avoid repetitive lumbar flexion/twisting. |
 A Microdiscectomy is usually performed as an outpatient procedure, allowing patients to go home the same day. First‑week postoperative care focuses on incision hygiene, pain control, and limited movement. Keep the wound clean and dry, avoid hydrogen peroxide or alcohol, and change dressings only as directed. Bending, twisting and lifting should not exceed 5‑10 lb, and driving is avoided for at least two weeks. Short walks of 5‑10 minutes, 3‑4 times daily, promote circulation and reduce stiffness without over‑stress the surgical site.
A Microdiscectomy is usually performed as an outpatient procedure, allowing patients to go home the same day. First‑week postoperative care focuses on incision hygiene, pain control, and limited movement. Keep the wound clean and dry, avoid hydrogen peroxide or alcohol, and change dressings only as directed. Bending, twisting and lifting should not exceed 5‑10 lb, and driving is avoided for at least two weeks. Short walks of 5‑10 minutes, 3‑4 times daily, promote circulation and reduce stiffness without over‑stress the surgical site.
Week‑by‑week recovery milestones:
- Week 1: Rest, incision care, gentle ambulation.
- Week 2: Pain usually subsides; light household chores and low‑impact stretching may begin.
- Weeks 3‑5: Supervised physical therapy emphasizing core strengthening; continue avoiding heavy lifting.
- Week 6 onward: Gradual return to normal activities and office work; low‑impact aerobic exercise is safe. Heavy lifting and high‑impact sports are typically postponed until after week 12.
Walking recommendations: Start with short, frequent bouts; increase duration as tolerated. Excessive walking that provokes persistent pain, swelling, or renewed sciatica should be curtailed and discussed with the surgeon.
Permanent activity restrictions: Most patients resume daily life but should avoid heavy lifting (>10‑15 lb), high‑impact sports, and repetitive lumbar flexion or twisting. Proper body mechanics—bending at the knees and keeping a neutral spine—help protect the healed disc.
Overall recovery time: Many feel better within a few weeks, but full functional recovery is typically achieved between 8‑12 weeks, with a return to demanding activities by three months, depending on individual healing and adherence to rehabilitation.
Pain Management: Medications and Non‑Surgical Strategies
| Medication Type | Examples | Typical Use |
|---|---|---|
| NSAIDs | Ibuprofen, Naproxen, Diclofenac, Prescription‑strength ibuprofen | Reduce inflammation & mild‑moderate pain. |
| Opioids (short‑term) | Hydrocodone, Oxycodone, Tramadol | Severe radicular pain when OTC insufficient; close monitoring. |
| Muscle Relaxants | Cyclobenzaprine, Tizanidine, Methocarbamol | Alleviate spasm. |
| Neuropathic Agents | Duloxetine, Gabapentin, Pregabalin | Chronic nerve‑related pain. |
| Acetaminophen | Tylenol | Adjunct analgesic; safe for mild pain. |
| Non‑Pharm | Cold pack 15‑20 min → heat pad; knee‑to‑chest stretch, cat‑cow, short walks; posture correction; standing breaks. | Immediate inflammation control & muscle relaxation. |
| Female‑Specific | Emphasize core PT, posture, low‑impact cardio; consider hormonal influences; avoid high‑impact until pregnancy resolves. | Tailored to hormonal & anatomical factors. |
 When over‑the‑counter (OTC) options are insufficient, physicians may prescribe stronger NSAIDs—such as prescription‑strength ibuprofen, naproxen, or diclofenac—or short‑term opioids (hydrocodone, oxycodone, tramadol) under close monitoring. Muscle relaxants (cyclobenzaprine, tizanidine) are added for spasm, while low‑dose duloxetine or gabapentin address chronic neuropathic pain. Common back‑pain medications include acetaminophen (Tylenol), ibuprofen (Advil, Motrin), naproxen (Aleve), cyclobenzaprine (Flexeril), methocarbamol (Robaxin), and, for severe pain, oxycodone or hydrocodone. Antidepressants (duloxetine) and anticonvulsants (gabapentin, pregabalin) target nerve‑related symptoms.
When over‑the‑counter (OTC) options are insufficient, physicians may prescribe stronger NSAIDs—such as prescription‑strength ibuprofen, naproxen, or diclofenac—or short‑term opioids (hydrocodone, oxycodone, tramadol) under close monitoring. Muscle relaxants (cyclobenzaprine, tizanidine) are added for spasm, while low‑dose duloxetine or gabapentin address chronic neuropathic pain. Common back‑pain medications include acetaminophen (Tylenol), ibuprofen (Advil, Motrin), naproxen (Aleve), cyclobenzaprine (Flexeril), methocarbamol (Robaxin), and, for severe pain, oxycodone or hydrocodone. Antidepressants (duloxetine) and anticonvulsants (gabapentin, pregabalin) target nerve‑related symptoms.
Fast home relief: Apply a 15‑20‑minute cold pack to reduce inflammation, then a heating pad to relax muscles. Perform gentle stretches—knee‑to‑chest, cat‑cow—and short 5‑minute walks. Maintain good posture, take brief standing breaks each hour, and use OTC NSAIDs or acetaminophen as needed.
Instant techniques: A cold or heat pack for 15‑20 minutes, followed by a quick knee‑to‑chest stretch, can decompress the spine. Sit with shoulders back, roll a towel under the lower back, and practice slow, deep breathing to lower tension.
Female‑specific care: Begin with activity modification, heat/cold therapy, and NSAIDs. Emphasize core‑strengthening PT, posture correction, and low‑impact cardio. For persistent pain, minimally invasive options such as epidural steroid injections or endoscopic decompression are considered, with attention to hormonal changes and pregnancy‑related considerations.
Women’s Back Pain: Causes and Prevention
| Category | Common Causes | Prevention Tips |
|---|---|---|
| Orthopedic | Osteoarthritis, Spondylolisthesis, Sacroiliac joint dysfunction, Disc herniation (L4‑L5, L5‑S1). | Core‑strengthening (plank, bird‑dog, Pilates), ergonomic workstation, weight management. |
| Hormonal | Menstrual cycle, pregnancy, menopause → ligament laxity, bone density changes. | Calcium/Vitamin D, weight‑bearing exercise, posture awareness during pregnancy. |
| Gynecologic | Endometriosis, Pelvic inflammatory disease (referred pain). | Prompt gynecologic evaluation, pelvic floor PT. |
| Lifestyle | Prolonged sitting, poor ergonomics, weak core, smoking, excess weight. | Hourly walks, lumbar support, smoking cessation, regular low‑impact cardio. |
| Mind‑Body | Stress‑induced muscle tension. | Mindfulness, yoga, tai chi, deep‑breathing exercises daily |
 Women experience back pain for a unique blend of orthopedic, hormonal, and lifestyle reasons. Orthopedic contributors include common conditions such as osteoarthritis, spondylolisthesis, and sacroiliac joint dysfunction. A wider pelvis changes spinal curvature and places extra strain on the lumbar spine, while disc herniation—particularly at L4‑L5 and L5‑S1—can compress nerve roots and trigger sciatica. Hormonal fluctuations during menstrual cycles, pregnancy, and menopause affect ligament laxity and bone density, making the spine more vulnerable to strain. Gynecologic issues like endometriosis or pelvic inflammatory disease may also refer pain to the lower back. Lifestyle factors—prolonged sitting, poor ergonomic habits, weak core muscles, excess weight, and smoking—exacerbate these underlying problems.
Women experience back pain for a unique blend of orthopedic, hormonal, and lifestyle reasons. Orthopedic contributors include common conditions such as osteoarthritis, spondylolisthesis, and sacroiliac joint dysfunction. A wider pelvis changes spinal curvature and places extra strain on the lumbar spine, while disc herniation—particularly at L4‑L5 and L5‑S1—can compress nerve roots and trigger sciatica. Hormonal fluctuations during menstrual cycles, pregnancy, and menopause affect ligament laxity and bone density, making the spine more vulnerable to strain. Gynecologic issues like endometriosis or pelvic inflammatory disease may also refer pain to the lower back. Lifestyle factors—prolonged sitting, poor ergonomic habits, weak core muscles, excess weight, and smoking—exacerbate these underlying problems.
To reduce back pain, women should adopt a targeted prevention plan. Begin each day with gentle stretches (knee‑to‑chest, cat‑cow, bridge) to improve flexibility, then integrate core‑strengthening exercises such as planks, bird‑dogs, and Pilates‑based movements. Maintain an ergonomic workstation: sit with hips and knees at 90°, use lumbar support, and take short walks every hour. Aim for low‑impact cardio (walking, swimming, cycling) to promote circulation without overloading the spine. Keep a healthy weight, stay hydrated, and quit smoking to support bone health. Finally, consider mindfulness practices, yoga, or tai chi to lower inflammation and improve pain perception. Consistency with these habits can dramatically lower the risk of chronic back pain and improve overall spinal health.
Minimally Invasive Spine Surgery (MISS): Benefits, Downsides, and Evidence
| Aspect | Benefits | Downsides / Evidence |
|---|---|---|
| Incision & Tissue | ≤2 cm incision, tubular retractors preserve muscle & ligament; less postoperative pain. | Requires steep learning curve; specialized equipment. |
| Blood Loss & Infection | Significantly lower intra‑operative blood loss; reduced infection rates. | Rare complications: nerve injury, dural tear, hardware misplacement. |
| Hospital Stay | Outpatient or overnight stay; faster discharge. | Higher upfront technology costs; limited availability in some centers. |
| Recovery | Light duties return 2‑4 weeks; full work 6‑8 weeks. | Recurrence of disc herniation possible; need for future fusion in complex cases. |
| Evidence | Systematic reviews show comparable pain relief to open surgery with shorter LOS and lower opioid use. | Long‑term durability comparable to open; cost‑effectiveness balanced by reduced postoperative care. |
 MicroMinimally invasive spine surgery (MISS) is a modern approach that uses incisions no larger than 2 cm, tubular retractors, and high‑definition microscopes or endoscopes. By preserving muscle fibers and ligamentous structures, MISS dramatically reduces tissue trauma, blood loss, and infection risk. Patients typically leave the hospital the same day or after a brief overnight stay and can resume light daily activities within two to four weeks, with many returning to full work duties by six to eight weeks. These clinical advantages translate into faster functional recovery while maintaining spinal stability.
MicroMinimally invasive spine surgery (MISS) is a modern approach that uses incisions no larger than 2 cm, tubular retractors, and high‑definition microscopes or endoscopes. By preserving muscle fibers and ligamentous structures, MISS dramatically reduces tissue trauma, blood loss, and infection risk. Patients typically leave the hospital the same day or after a brief overnight stay and can resume light daily activities within two to four weeks, with many returning to full work duties by six to eight weeks. These clinical advantages translate into faster functional recovery while maintaining spinal stability.
Downside – Despite its minimally disruptive nature, MISS is not without risk. Rare but serious complications include nerve injury, dural tears (spinal fluid leaks), and, in complex cases, hardware misplacement or recurrence of disc herniation. The steep learning curve for surgeons and the need for advanced imaging and navigation technology can increase operative costs and limit availability in some settings.
Evidence from PubMed – Recent systematic reviews and large cohort studies confirm that MISS provides pain relief and functional outcomes comparable to traditional open surgery, but with significantly lower intra‑operative blood loss, shorter hospital stays, and reduced postoperative infection rates. Cost‑effectiveness analyses show that the higher upfront technology expense is offset by decreased postoperative care and faster return to productivity.
Surgical techniques and disease management – MISS encompasses a suite of procedures: percutaneous pedicle‑screw fixation, tubular decompression, endoscopic microdiscectomy, and lateral‑transpsoas interbody fusion. Intra‑operative CT, navigation, and neuromonitoring enhance precision, allowing effective treatment of lumbar disc herniation, spinal stenosis, spondylolisthesis, and select tumors while preserving native anatomy. This patient‑first, minimally invasive philosophy aligns with our practice’s commitment to rapid, safe, and durable spine care.
Cost, Insurance, and Decision‑Making in Spine Care
| Cost Component | Typical Range (USD) | Notes |
|---|---|---|
| Surgeon Fees | $5 000 – $20 000 | Varies by surgeon experience & region. |
| Hospital Charges | $10 000 – $30 000 | Includes OR time, facility fees. |
| Anesthesia | $1 000 – $3 000 | Depends on duration & anesthesiologist. |
| Imaging | $500 – $2 000 | Pre‑op MRI/CT, intra‑op fluoroscopy. |
| Post‑Op PT | $1 000 – $5 000 | Typically 6‑12 weeks of therapy. |
| Insurance Coverage | Medicare & most major insurers cover when medically necessary after 6‑12 weeks of conservative care. | Patients responsible for deductibles, copays, coinsurance. |
| Decision‑Making | Exhaust non‑surgical measures first; consider surgery if radicular pain persists and functional loss. | Weigh short‑term benefits of microdiscectomy vs. potential need for future fusion. |
 Microdiscectomy is a common minimally invasive option for lumbar disc herniation, and its cost can be a deciding factor for many patients. In the United States the total expense typically ranges from $20,000 to $50,000, broken down into surgeon fees ($5‑$20 k), hospital charges ($10‑$30 k), anesthesia ($1‑$3 k), imaging ($0.5‑$2 k) and postoperative physical therapy ($1‑$5 k). Most major insurers, including Medicare, will cover a microdiscectomy when it is deemed medically necessary after a documented trial of 6‑12 weeks of conservative care, but patients are still responsible for deductibles, copays, and coinsurance.
Microdiscectomy is a common minimally invasive option for lumbar disc herniation, and its cost can be a deciding factor for many patients. In the United States the total expense typically ranges from $20,000 to $50,000, broken down into surgeon fees ($5‑$20 k), hospital charges ($10‑$30 k), anesthesia ($1‑$3 k), imaging ($0.5‑$2 k) and postoperative physical therapy ($1‑$5 k). Most major insurers, including Medicare, will cover a microdiscectomy when it is deemed medically necessary after a documented trial of 6‑12 weeks of conservative care, but patients are still responsible for deductibles, copays, and coinsurance.
When evaluating surgery, clinicians advise patients to first exhaust non‑surgical measures because many disc herniations improve with activity modification, NSAIDs, and targeted physical therapy. Surgery carries low‑frequency risks such as infection, nerve injury, dural tears, and the possibility of failed‑back‑surgery syndrome; recurrence or scar tissue can also develop. For those with persistent radicular pain despite these measures, microdiscectomy offers a high success rate (70‑90 % leg‑pain relief) and a rapid return to function.
Long‑term outcomes of minimally invasive spinal fusion (MISF) compare favorably with traditional open fusion. Both achieve similar fusion rates and sustained pain relief, but MISF typically results in less blood loss, shorter hospital stays, and lower infection rates, making it more cost‑effective while preserving durability. Consequently, patients and surgeons weigh the short‑term benefits of a microdiscectomy against the potential need for future fusion, always prioritizing evidence‑based, patient‑first care.
Patient‑First Care at the Orthopedic Spine Institute of St. Louis
| Step | Description |
|---|---|
| 1. Comprehensive Evaluation | Detailed history, neurological exam, high‑resolution MRI/CT to pinpoint pain source. |
| 2. Conservative First | Physical therapy, NSAIDs, epidural injections before any surgical recommendation. |
| 3. Surgical Indication | If conservative care fails, minimally invasive microdiscectomy is preferred. |
| 4. Patient Education | Access to videos explaining anatomy, procedure steps, and rehab protocols. |
| 5. Personalized Treatment Plan | Tailored to patient’s lifestyle goals, health status, and insurance considerations. |
| 6. Follow‑Up & Rehab | Structured post‑op PT, activity guidelines, and ongoing support from spine‑care coordinator. |
 At the Orthopedic Spine Institute of St. Louis, every new patient begins with a comprehensive evaluation that blends detailed history‑taking, focused neurological exam, and high‑resolution imaging (MRI or CT) to pinpoint the exact source of back or leg pain. Dr. David S. Raskas’s philosophy centers on a "patient‑first" approach: conservative care—physical therapy, medication, epidural injections—must be exhausted before any surgical recommendation, and when surgery is indicated, minimally invasive spine surgery (MISS) is the preferred option.
At the Orthopedic Spine Institute of St. Louis, every new patient begins with a comprehensive evaluation that blends detailed history‑taking, focused neurological exam, and high‑resolution imaging (MRI or CT) to pinpoint the exact source of back or leg pain. Dr. David S. Raskas’s philosophy centers on a "patient‑first" approach: conservative care—physical therapy, medication, epidural injections—must be exhausted before any surgical recommendation, and when surgery is indicated, minimally invasive spine surgery (MISS) is the preferred option.
MISS utilizes small ( ≤2 cm) incisions, tubular retractors, and real‑time fluoroscopic or endoscopic visualization to remove herniated disc fragments while preserving muscle and ligament integrity. This technique yields lower blood loss, reduced postoperative pain, shorter hospital stays (often outpatient), and a faster return to daily activities compared with traditional open procedures.
The Institute equips patients with educational resources, including videos that explain the anatomy of a herniated disc, the step‑by‑step microdiscectomy process, and postoperative rehabilitation protocols. These tools empower patients to make informed decisions and set realistic expectations for recovery.
To start the journey, contact the Institute’s spine‑care coordinator for a pre‑screening questionnaire, schedule a consultation with Dr. Raskas, and receive a personalized treatment plan that prioritizes safety, efficacy, and the patient’s lifestyle goals.
Putting the Facts Together for Informed Spine Decisions
Microdiscectomy is a minimally invasive, evidence‑based option for patients with sciatica caused by a single‑level lumbar disc herniation that has not improved after 6–12 weeks of physical therapy, NSAIDs, or epidural steroid injections. Modern techniques use a 1‑2 cm incision, a microscope or endoscope, and tubular retractors, preserving muscle and ligament integrity. Success rates are high—70‑90 % of patients experience meaningful leg‑pain relief within weeks, and most can return to light office work in 2‑4 weeks and to normal activities by 6‑8 weeks. Complication rates are low (≤2 % for dural tears, infection, or nerve injury), and the procedure avoids the hardware and longer recovery associated with spinal fusion. However, outcomes depend on careful patient selection, imaging confirmation of disc‑root correlation, and optimization of modifiable risk factors such as smoking, diabetes, and obesity.
Because each spine condition is unique, a personalized, evidence‑driven approach is essential. Dr. David S. Raskas at the Orthopedic Spine Institute of St. Louis conducts thorough clinical and imaging evaluations, discusses realistic expectations, and tailors postoperative rehabilitation—including core‑strengthening and low‑impact aerobic exercise—to support long‑term spinal health. Schedule a consultation with Dr. Raskas to determine whether microdiscectomy fits your specific situation and to develop a recovery plan that maximizes pain relief while minimizing downtime.
