Understanding Spinal Decompression and Laminectomy
Spinal decompression surgery creates space for compressed nerves by removing bone, ligament, or disc material; a laminectomy is a specific type of decompression that surgically removes the lamina, the protective “roof” of a vertebra, to enlarge the spinal canal. The most common indications include lumbar spinal stenosis, herniated discs, bone spurs, spondylolisthesis, and neurogenic claudication that cause leg pain, numbness, weakness, or gait difficulty after conservative treatments have failed. At the Orthopedic Spine Institute of St. Louis, a patient‑first philosophy guides every step: thorough non‑surgical evaluation, personalized imaging review, smoking‑cessation and fitness counseling, and discussion of minimally invasive options before considering open surgery. This approach ensures patients receive the least invasive, most effective treatment tailored to their unique anatomy and lifestyle, optimizing outcomes and satisfaction.
Why Surgery May Be Needed – From Home Care to Operative Solutions
Conservative Care vs Surgical Indication
| Aspect | Conservative Care | Surgical Indication |
|---|---|---|
| Pain control | Ice 20 min qid, NSAIDs, gentle activity | Persistent pain >6‑12 wk despite therapy |
| Mobility | Short walks, light stretches | Worsening leg pain, numbness, weakness |
| Red‑flags | None | New bladder/bowel loss, fever, incision drainage |
| Imaging | Usually not needed | Significant canal narrowing on MRI/CT |
| Timeline | 6‑12 wk trial | Failure of conservative trial or red‑flag present |
 Initial self‑care strategies focus on pain control and gentle movement. Apply an ice pack for 20 minutes several times a day during the first 48 hours, then switch to a heating pad for another 20‑minute session to reduce inflammation and relax tight muscles. Take an over‑the‑counter NSAID such as ibuprofen as directed, and combine it with low‑impact activity like short walks to keep blood flowing. Simple home stretches—knees‑to‑chest, lower‑back rotational stretch, cat‑cow, and a brief bridge—hold each for 5‑10 seconds and repeat 2‑3 times twice daily. Maintain good posture and take brief movement breaks every hour.
Initial self‑care strategies focus on pain control and gentle movement. Apply an ice pack for 20 minutes several times a day during the first 48 hours, then switch to a heating pad for another 20‑minute session to reduce inflammation and relax tight muscles. Take an over‑the‑counter NSAID such as ibuprofen as directed, and combine it with low‑impact activity like short walks to keep blood flowing. Simple home stretches—knees‑to‑chest, lower‑back rotational stretch, cat‑cow, and a brief bridge—hold each for 5‑10 seconds and repeat 2‑3 times twice daily. Maintain good posture and take brief movement breaks every hour.
Red‑flag symptoms that should prompt immediate medical attention include new or worsening leg pain, numbness, weakness, loss of bladder or bowel control, fever, swelling, redness, or drainage from the incision. These signs may indicate infection, nerve injury, or spinal instability that requires urgent evaluation.
Criteria for moving from conservative to operative treatment involve persistent nerve‑compression symptoms (e.g., radiculopathy, neurogenic claudication) that do not improve after 6–12 weeks of physical therapy, NSAIDs, and injections, and imaging that confirms significant spinal canal narrowing. When these thresholds are met, a laminectomy—open or minimally invasive—can be offered to relieve pressure on the spinal cord or nerve roots and restore function.
L4‑L5 Decompression and Fusion – What to Expect
Procedure Overview
| Item | Details |
|---|---|
| Technique | Mini‑incision laminectomy/laminotomy + micro‑discectomy; fluoroscopy & tubular retractors |
| Hospital stay | 1‑4 days (same‑day for simple decompression) |
| Early ambulation | Walk day of surgery |
| Return to light work | 4‑6 weeks |
| Return to heavy work / full activity | 3‑6 months (fusion) |
| Success rate (relief) | 70‑80 % of patients |
| Patient satisfaction | up to 90 % |
| Complication rate | 2‑5 % in experienced centers |
 A minimally invasive L4‑L5 decompression combines a small‑incision laminectomy or laminotomy with micro‑discectomy to remove bone, ligament or herniated disc material that compresses the nerve roots at the fourth‑and‑fifth lumbar levels. Real‑time fluoroscopy and tubular retractors preserve muscle tissue, resulting in less blood loss and faster healing. Most patients walk the day of surgery and are discharged after 1‑4 days, often the same day for a simple decompression and up to two days when a fusion is added. Clinical data show that 70‑80 % of patients experience marked relief of sciatica, leg pain and numbness, with up to 90 % reporting satisfaction when the procedure is successful. Risks remain low but include infection, blood clots, nerve injury, dural tears and rare spinal‑cord damage; complication rates in experienced centers hover around 2‑5 %. Recovery timelines differ: isolated decompression allows light activity in 1‑2 weeks and full work by 4‑6 weeks, while an accompanying minimally invasive fusion extends return to normal activities to 3‑6 months. Adherence to postoperative guidelines, smoking cessation and a structured physical‑therapy program are essential for optimal long‑term outcomes.
A minimally invasive L4‑L5 decompression combines a small‑incision laminectomy or laminotomy with micro‑discectomy to remove bone, ligament or herniated disc material that compresses the nerve roots at the fourth‑and‑fifth lumbar levels. Real‑time fluoroscopy and tubular retractors preserve muscle tissue, resulting in less blood loss and faster healing. Most patients walk the day of surgery and are discharged after 1‑4 days, often the same day for a simple decompression and up to two days when a fusion is added. Clinical data show that 70‑80 % of patients experience marked relief of sciatica, leg pain and numbness, with up to 90 % reporting satisfaction when the procedure is successful. Risks remain low but include infection, blood clots, nerve injury, dural tears and rare spinal‑cord damage; complication rates in experienced centers hover around 2‑5 %. Recovery timelines differ: isolated decompression allows light activity in 1‑2 weeks and full work by 4‑6 weeks, while an accompanying minimally invasive fusion extends return to normal activities to 3‑6 months. Adherence to postoperative guidelines, smoking cessation and a structured physical‑therapy program are essential for optimal long‑term outcomes.
Cost Landscape – From Open to Minimally Invasive Techniques
Cost Comparison (U.S.)
| Procedure | Insured out‑of‑pocket | Uninsured out‑of‑pocket | Avg operating cost |
|---|---|---|---|
| Open diskectomy | $15‑35 k | $15‑35 k | $27 k |
| Open laminectomy | $15‑35 k | $50‑90 k | $27 k |
| Open fusion | $80‑150 k | >$150 k | $27 k |
| MIS diskectomy | $10‑30 k | $15‑35 k | $24.3 k |
| MIS fusion | $10‑30 k | $80‑150 k | $24.3 k |
| Non‑surgical therapy (course) | $1‑5 k | $30‑200 per session | – |
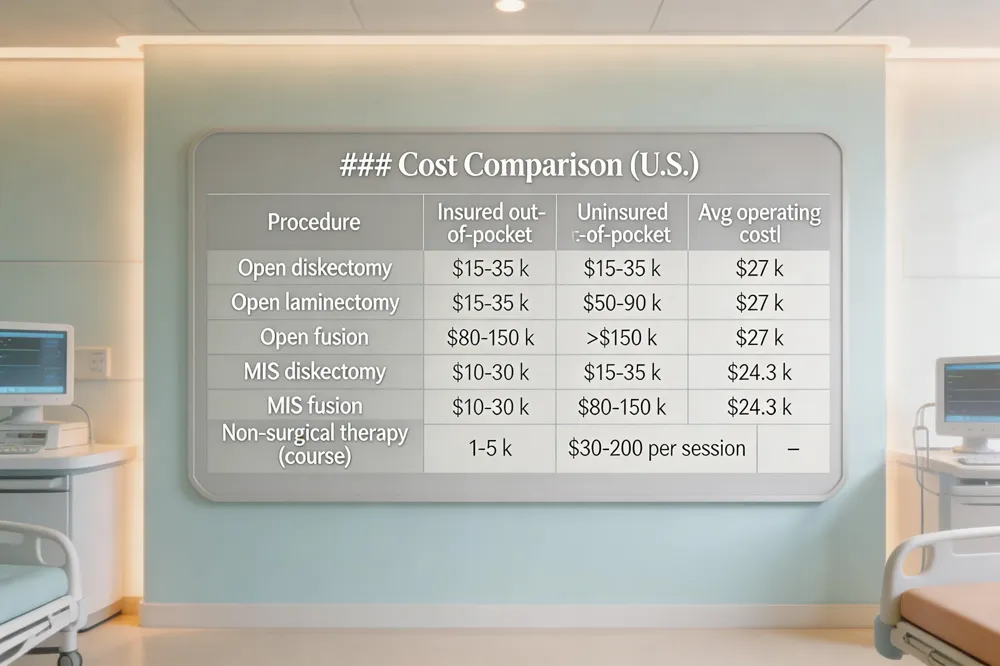 Spinal decompression surgery in the U.S. typically runs $8,000‑$25,000 out‑of‑pocket after insurance; without coverage the bill can soar to $15,000‑$35,000 for a diskectomy and $50,000‑$90,000 for a laminectomy, while extensive fusions may exceed $150,000. Non‑surgical decompression therapy is $30‑$200 per session, usually $1,000‑$5,000 for a full course.
Spinal decompression surgery in the U.S. typically runs $8,000‑$25,000 out‑of‑pocket after insurance; without coverage the bill can soar to $15,000‑$35,000 for a diskectomy and $50,000‑$90,000 for a laminectomy, while extensive fusions may exceed $150,000. Non‑surgical decompression therapy is $30‑$200 per session, usually $1,000‑$5,000 for a full course.
Minimally invasive spine surgery (MIS) often costs less than open procedures because hospital stays are shorter and recovery quicker. Insured patients generally see $10,000‑$30,000 out‑of‑pocket, compared with $15,000‑$35,000 for open diskectomy or $80,000‑$150,000 for fusion without coverage. Average MIS lumbar fusion operating costs are $24,300 versus $27,100 for the open approach, a saving of roughly $2,800 (≈10%).
Downsides of MIS include anesthesia reactions, blood clots, infection, limited visual fields that can cause nerve or dural injury, and a learning curve for surgeons that may increase conversion to open surgery or need for revision.
Our institute provides dedicated financial counseling to verify insurance benefits, explore payment plans, and minimize unexpected expenses.
Recovery Pathways – From Hospital Discharge to Full Activity
Recovery Timeline by Procedure
| Procedure | Hospital stay | First ambulation | Light work | Heavy work / driving | Full activity |
|---|---|---|---|---|---|
| L5‑S1 laminectomy | 1‑3 days | 2‑4 weeks | 4‑6 weeks | 8‑12 weeks | 8‑12 weeks |
| L4‑L5 laminectomy | 1‑4 days | 2‑4 weeks | 4‑6 weeks | 8‑12 weeks | 8‑12 weeks |
| MIS decompression | 1‑2 days | 1‑2 weeks | 2‑4 weeks | 2‑3 weeks | 6‑8 weeks |
| MIS fusion | 1‑2 days | 1‑2 weeks | 2‑4 weeks | 3‑4 weeks | 3‑6 months |
| Open fusion | 2‑4 days | 2‑4 weeks | 4‑8 weeks | 8‑12 weeks | 6‑12 months |
 Recovery after spinal decompression follows a predictable pattern, but timelines differ by procedure and level. Most patients overnight 1–3 days after an L5‑S1 laminectomy; light walking and gentle movements can start within 2–4 weeks, desk‑job work returns at 4–6 weeks, and full‑duty or heavy‑lifting jobs need 8–12 weeks. A structured Physical therapy program—focusing on core stabilization, gradual stretching, and gait training—is essential for regaining strength and mobility. For a L4‑L5 lumbar laminectomy, hospital stay is 1–4 days, with similar early ambulation. Heavy lifting, strenuous exercise, and driving are avoided for the first 2–4 weeks; sedentary work often resumes by 2–4 weeks, while more demanding jobs may require 4–8 weeks. Full activity typically returns by 8–12 weeks. Spinal decompression surgery (including laminectomy, laminotomy, or discectomy) usually involves a 1–2‑day stay. The first few weeks emphasize gentle walking and basic stretching; Physical therapy begins around week 2‑3. Pain and function improve markedly by 4–6 weeks, allowing return to sedentary work, while full‑strength exercise and high‑impact activities are usually safe at 3‑4 months. Recovery can range from 3 months for uncomplicated cases to 6 months when fusion is added. Minimally invasive spine surgery (MISS) shortens these intervals: patients often walk and stretch within 1‑2 weeks and may drive or work by the end of week 2. Full functional recovery for MISS laminectomy or microdiscectomy typically occurs in 6‑8 weeks; minimally invasive fusions need 3‑6 months, with a 3‑4‑week “lay‑up” phase before vigorous activity. Across all techniques, adherence to surgeon‑directed activity restrictions, wound care, and a progressive rehabilitation program maximizes outcomes and minimizes complications.
Recovery after spinal decompression follows a predictable pattern, but timelines differ by procedure and level. Most patients overnight 1–3 days after an L5‑S1 laminectomy; light walking and gentle movements can start within 2–4 weeks, desk‑job work returns at 4–6 weeks, and full‑duty or heavy‑lifting jobs need 8–12 weeks. A structured Physical therapy program—focusing on core stabilization, gradual stretching, and gait training—is essential for regaining strength and mobility. For a L4‑L5 lumbar laminectomy, hospital stay is 1–4 days, with similar early ambulation. Heavy lifting, strenuous exercise, and driving are avoided for the first 2–4 weeks; sedentary work often resumes by 2–4 weeks, while more demanding jobs may require 4–8 weeks. Full activity typically returns by 8–12 weeks. Spinal decompression surgery (including laminectomy, laminotomy, or discectomy) usually involves a 1–2‑day stay. The first few weeks emphasize gentle walking and basic stretching; Physical therapy begins around week 2‑3. Pain and function improve markedly by 4–6 weeks, allowing return to sedentary work, while full‑strength exercise and high‑impact activities are usually safe at 3‑4 months. Recovery can range from 3 months for uncomplicated cases to 6 months when fusion is added. Minimally invasive spine surgery (MISS) shortens these intervals: patients often walk and stretch within 1‑2 weeks and may drive or work by the end of week 2. Full functional recovery for MISS laminectomy or microdiscectomy typically occurs in 6‑8 weeks; minimally invasive fusions need 3‑6 months, with a 3‑4‑week “lay‑up” phase before vigorous activity. Across all techniques, adherence to surgeon‑directed activity restrictions, wound care, and a progressive rehabilitation program maximizes outcomes and minimizes complications.
Complications, Long‑Term Effects and Lifestyle Adjustments
Complications & Adjustments
| Complication | Early risk | Long‑term effect | Lifestyle adjustment |
|---|---|---|---|
| Infection | 2‑5 % | May require antibiotics / debridement | Wound care, monitor temperature |
| Dural tear / CSF leak | Intra‑op | Headache, possible meningitis | Bed rest, possible re‑op |
| Nerve injury | Intra‑op | Persistent numbness/weakness | Avoid heavy lifting, targeted PT |
| Epidural fibrosis | Months‑years | Chronic radicular pain | Structured PT, possible injections |
| Adjacent‑segment degeneration | Years | New pain at neighboring levels | Activity modification, periodic imaging |
| Post‑laminectomy syndrome | Variable | Ongoing pain, possible opioid use | Long‑term pain management plan |
 Laminectomy complications include infection, excessive bleeding, and postoperative blood clots that can impede healing. Nerve‑related injuries such as dural tears, cerebrospinal‑fluid leaks, or direct nerve‑root damage may cause numbness, weakness, or even cauda equina syndrome. Removing the lamina can also destabilize the spine, sometimes necessitating a secondary fusion. Scar‑tissue (epidural fibrosis) may produce persistent or recurrent pain and new neurological symptoms, especially in patients who smoke, have osteoporosis, or have undergone prior spine surgery.
Laminectomy complications include infection, excessive bleeding, and postoperative blood clots that can impede healing. Nerve‑related injuries such as dural tears, cerebrospinal‑fluid leaks, or direct nerve‑root damage may cause numbness, weakness, or even cauda equina syndrome. Removing the lamina can also destabilize the spine, sometimes necessitating a secondary fusion. Scar‑tissue (epidural fibrosis) may produce persistent or recurrent pain and new neurological symptoms, especially in patients who smoke, have osteoporosis, or have undergone prior spine surgery.
Long‑term side effects can involve persistent or recurrent back or neck pain—often termed failed‑back‑surgery syndrome. Post‑laminectomy instability may lead to abnormal motion or vertebral collapse, and adjacent‑segment degeneration is common as the levels above or below the operative site wear more quickly. [Epidural fibrosis can tether nerve roots, causing chronic radiating pain or numbness](https://my.clevelandclinic.org/health/treatments/10874-spinal-decompression-therapy) and some patients may develop long‑term opioid dependence.
Permanent activity restrictions after a simple [laminectomy](https://my.clevelandclinic.org/health/procedures/10895-laminectomy) without fusion are modest: lifelong avoidance of very heavy lifting (generally >10 lb) and repetitive high‑impact or jarring activities is advised, along with limiting sharp bending or twisting at the waist. If a fusion or hardware was added, restrictions are stricter and may require ongoing physical‑therapy guidance.
Buttock pain after [laminectomy](https://my.clevelandclinic.org/health/procedures/10895-laminectomy) often signals post‑laminectomy syndrome or piriformis irritation of the sciatic nerve. Initial management includes gentle stretching, targeted physical‑therapy exercises, and anti‑inflammatory medication. Persistent pain may require epidural steroid injections, nerve‑stimulating therapies, or, in select cases, revision surgery under the care of a spine specialist.
Optimizing Outcomes – Pain Management, Exercises and Patient Selection
Optimizing Outcomes
| Domain | Key Points |
|---|---|
| Pain management | OTC NSAIDs first; short‑term opioids (≤2 weeks) only for severe pain; monitor for dependence |
| Exercise phases | Weeks 0‑2: walking, pelvic tilt, knee‑to‑chest; Weeks 2‑6: core activation, diaphragmatic breathing, glides, bridges, bird‑dog; Weeks 6‑12: straight‑leg raises, wall squats, resistance bands |
| Patient selection for MIS | Ideal: non‑obese, non‑smoker, good bone quality, limited comorbidities; Poor candidates: severe osteoporosis, uncontrolled diabetes, heavy smoking, need extensive reconstruction |
| Post‑op tips | Wear lumbar brace if prescribed, change position every 30 min, maintain hydration & balanced diet, attend all PT sessions |
 Strong painkillers for lower‑back pain, such as prescription opioids (oxycodone, hydrocodone, morphine or tramadol), are reserved for severe, short‑term pain that has not responded to milder agents like acetaminophen, NSAIDs or muscle‑relaxants. Because of the high risk of dependence, constipation, drowsiness and respiratory depression, surgeons prescribe the lowest effective dose for no longer than one to two weeks and monitor closely.
Strong painkillers for lower‑back pain, such as prescription opioids (oxycodone, hydrocodone, morphine or tramadol), are reserved for severe, short‑term pain that has not responded to milder agents like acetaminophen, NSAIDs or muscle‑relaxants. Because of the high risk of dependence, constipation, drowsiness and respiratory depression, surgeons prescribe the lowest effective dose for no longer than one to two weeks and monitor closely.
Laminectomy recovery exercises begin with gentle walking and pelvic‑tilt or knee‑to‑chest stretches to promote circulation while the incision heals. In the first weeks focus on deep‑abdominal activation and diaphragmatic breathing, then progress to neural glides, clamshells, drawing‑in maneuvers, dead‑bug, bridges and bird‑dog. By three to six weeks, add straight‑leg raises, prone press‑ups, wall squats, side‑lying hip abductions and light resistance‑band work as pain permits and the surgeon clears weight‑bearing activities.
People who achieve relief with non‑surgical care, have severe osteoporosis, uncontrolled diabetes or cardiovascular disease, are obese, heavy smokers, or require extensive spinal reconstruction are not ideal candidates for minimally invasive spine surgery.
Recovery tips include following the surgeon’s activity schedule, using a lumbar brace if prescribed, limiting lifting to light objects, changing position every 30 minutes, attending all physical‑therapy sessions, and maintaining a balanced diet with adequate hydration to support tissue healing and reduce infection risk.
Frequently Asked Questions – Quick Answers for Patients
FAQ Summary
| Question | Answer |
|---|---|
| How long does it take to heal from a laminectomy? | Full recovery 3‑6 months; most notice major improvement by 6‑8 weeks |
| How bad is the pain after a laminectomy? | Moderate‑to‑severe first 1‑2 weeks, then eases; managed with meds, ice, gentle movement |
| What can you never do again after a laminectomy? | Avoid heavy lifting (>10 lb), high‑impact sports, prolonged driving without breaks, and excessive twisting at the waist |
| What is the hardest back surgery to recover from? | Spinal fusion, due to bone healing and motion restriction |
| Does lamina grow back after laminectomy? | Only limited new bone forms; original shape does not regenerate |
| How many years does a laminectomy last? | Typical relief 5‑10 years; durability varies, some need revision after a decade |
| What is the downside of laminectomy? | Risks: infection, bleeding, nerve injury, possible instability, prolonged rehab |
| What is the downside of minimally invasive spine surgery? | Anesthesia risks, blood clots, infection, limited visual field, learning‑curve for surgeons |
| How to get rid of back pain instantly? | Gentle stretch or short walk, ice for first 48 h then heat, correct posture, OTC NSAIDs; follow‑up for lasting relief |
 How short does it take to heal from a laminectomy? Full recovery usually spans 3‑6 months; the first 6‑8 weeks bring the most noticeable relief. Patients can sit and walk the day of surgery, and by 4‑6 weeks gait steadies and leg pain diminishes. Physical therapy restores strength, and most return to normal activities by three months, though some need up to six.
How short does it take to heal from a laminectomy? Full recovery usually spans 3‑6 months; the first 6‑8 weeks bring the most noticeable relief. Patients can sit and walk the day of surgery, and by 4‑6 weeks gait steadies and leg pain diminishes. Physical therapy restores strength, and most return to normal activities by three months, though some need up to six.
How bad is the pain after a laminectomy? Moderate‑to‑severe discomfort is common for the first 1‑2 weeks, managed with prescribed analgesics, ice, and gentle movement. Pain usually eases by weeks 3‑4; persistent pain may signal scar tissue or incomplete decompression and should prompt a surgeon’s review.
What can you never do again after a laminectomy? Heavy lifting, high‑impact sports, and prolonged driving without breaks are generally avoided indefinitely unless cleared; bending or twisting at the waist is restricted for several weeks.
What is the hardest back surgery to recover from? Spinal fusion, because it demands bone healing and extensive motion restriction.
Does lamina grow back after laminectomy? Only limited new bone forms; the original laminar shape does not regenerate, so stability relies on remaining tissues and any fusion hardware.
How many years does a laminectomy last? Most patients enjoy 5‑10 years of relief; durability varies with condition, technique, and rehab, and some may need revision after a decade.
What is the downside of laminectomy? Risks include infection, bleeding, nerve injury, and possible spinal instability requiring later fusion; persistent pain and a lengthy rehab are also possible.
What is the downside of minimally invasive spine surgery? Although less tissue‑disruptive, it still carries anesthesia risks, blood loss, infection, limited visual field, and a learning‑curve for surgeons that can lead to conversion to open surgery.
How to get rid of back pain instantly? Begin with gentle stretches or a short walk, apply ice for 48 hours then heat, correct posture, and use OTC NSAIDs as directed. For lasting relief, schedule a follow‑up with Dr. Raskas.
Moving Forward with Confidence
At our clinic we put you first, listening to your story and goals. A personalized plan blends your imaging, health history, and lifestyle to choose the right decompression technique—open or minimally invasive. Ready to take the next step? Schedule a consultation, bring your imaging, and let our expert team map a safe, effective path to relief and long‑term wellbeing today.
